
This impact is especially significant in high-volume settings, where even small variations in closure technique can affect workflow efficiency.
Studies show that staplers can reduce closure time by up to 66.6% compared with sutures, while providing cosmetic outcomes comparable to sutures in selected cases.
To simplify this process, skin staplers are commonly used, providing a faster, more standardized method of wound approximation.
In this blog, you’ll explore what a skin stapler is, how it functions during closure, and its most appropriate applications, with a focus on practical use and surgical decision-making.
Key Takeaways:
- Skin staplers enable rapid, consistent wound closure by mechanically approximating skin edges with a single-step activation.
- Staple formation into a “B-shaped” configuration supports stable tissue alignment with controlled edge eversion.
- Commonly used across surgical and emergency settings, particularly for linear incisions where speed and efficiency are priorities.
- Closure outcomes depend on proper technique, patient selection, and appropriate wound characteristics rather than the device alone.
- Consistent spacing, perpendicular placement, and correct edge eversion are critical to achieving reliable healing and minimizing complications.
What Is a Skin Stapler?
A skin stapler is a handheld surgical device designed to close wounds by mechanically deploying metal staples through both skin edges.
When activated, the device inserts and forms a staple that approximates wound edges in a single step. This enables:
- Rapid tissue approximation: Each activation delivers a formed staple in a single step
- Consistent staple geometry: Uniform formation supports predictable edge alignment
- Mechanical edge eversion: Helps maintain proper wound edge positioning when applied correctly
While innovation continues to refine stapling technology, clinical outcomes remain central to evaluating its effectiveness.
Real Case Study
In a comparative study of 100 patients undergoing abdominal wound closure, 50 patients received skin staples while 50 were treated with conventional sutures.
The study evaluated healing outcomes, infection rates, and overall wound characteristics across both groups.
- 76% of patients in the stapler group showed normal wound healing
- 24% experienced wound infections following stapled closure
In comparison, 88% of patients in the suture group achieved normal healing, with only 12% developing infections.
Despite differences in healing outcomes, staplers were associated with reduced closure time, making them a practical choice in high-volume surgical settings.
Findings such as these also highlight the importance of selecting the appropriate stapler type for each surgical context.
Key Types of Skin Staplers
Skin staplers vary in design, tissue compatibility, and clinical applications. Selecting the appropriate type depends on the surgical context and closure requirements.

After clarifying what a skin stapler is, it’s helpful to look at how the mechanism works in real surgical settings.
How Does a Skin Stapler Work?
Skin staplers close wounds through a mechanical process that delivers and forms a staple in a single trigger action. The device is designed to approximate wound edges quickly and consistently while maintaining controlled tissue compression.
To understand this process, it helps to break down the key steps involved during staple placement:
1. Loading and Positioning
Modern skin staplers are preloaded with sterile metal staples, typically made from stainless steel or titanium. The device is positioned perpendicular to the wound, with the surgeon ensuring proper alignment and slight eversion of the wound edges before firing.
Accurate positioning at this stage is critical, as edge alignment directly influences closure quality and healing outcomes.
2. Staple Deployment and Penetration
When the handle is activated, the stapler drives a staple through both edges of the skin. The staple penetrates the epidermis and dermis simultaneously, anchoring the tissue at two points on either side of the incision.
This single-step deployment allows for rapid closure and reduces the number of manual steps compared to suturing.
3. Staple Formation and Closure
As the staple passes through the tissue, it contacts the anvil within the device. The anvil bends the staple legs inward, forming a rectangular or “B-shaped” configuration that secures the wound edges together.
This formed shape supports stable tissue approximation and controlled edge eversion, which are important for proper healing.
The mechanism also avoids excessive compression of surrounding tissue while maintaining consistent closure across the incision. In practice, this results in:
- Stable edge approximation: Maintains alignment across the wound length
- Controlled eversion: Supports favorable healing conditions when applied correctly
- Consistent mechanical closure: Reduces variability compared to manual techniques
Traditional metal staples achieve this through external fixation on the skin surface, whereas subcuticular systems place fasteners beneath the skin to approximate the dermal layer without penetrating the skin.
In longer incisions, where closure time and consistency become more critical, subcuticular systems such as SubQ It! SU-25 extends this concept by enabling rapid dermal approximation while eliminating the need for a separate staple removal step.
4. Staple Release and Finalization
After formation, the stapler releases the staple and resets for the next deployment. The surgeon then assesses placement, ensuring:
- Proper staple formation: Fully formed “box” shape
- Adequate spacing: Typically several millimeters between staples, depending on wound characteristics
- Secure approximation: Wound edges aligned without excessive tension
This process is repeated along the incision until complete closure is achieved.
The way a skin stapler operates directly influences the settings in which it is most commonly used.
3 Key Applications of Skin Staplers in 2026
Skin staplers are primarily used to close linear skin wounds when rapid approximation is required, and tissue tension is manageable. Their use spans elective, emergency, and trauma settings, particularly in procedures where speed and consistency are critical.
To understand their role in practice, it is important to review where staplers are most commonly applied in 2026:
1. Primary Surgical Applications
Skin staplers are widely used across multiple surgical specialties for routine incision closure.
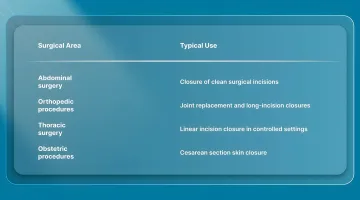
Staplers are commonly used in these cases because they allow faster closure than sutures, particularly in longer incisions, while maintaining consistent approximation.
2. Emergency and Trauma Settings
In emergency care, staplers are frequently used where rapid wound closure is necessary and time is a limiting factor. Their simplicity and speed make them particularly useful in high-throughput or acute care environments.
Typical emergency indications include:
- Scalp lacerations: Rapid closure in emergency departments
- Pediatric lacerations: Faster application reduces procedure time
- Trauma scenarios: Temporary or definitive closure in urgent settings
- Mass casualty situations: Efficient wound management under time pressure
3. Specialty and Emerging Applications
While traditionally used for speed rather than cosmetic precision, staplers are also applied in select specialized scenarios:
- Skin graft fixation: Securing grafts in reconstructive procedures
- Adjunct wound management: Supporting temporary closure or reinforcement
While these applications highlight where skin staplers are commonly used, proper technique remains equally important.
5 Things to Keep In Mind While Using Skin Staplers
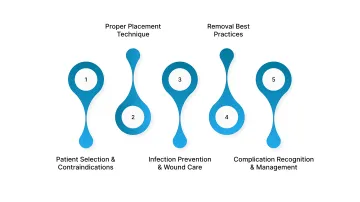
Skin staplers are widely used in surgical closure, but outcomes depend heavily on proper patient selection, technique, and postoperative management. Attention to these factors helps reduce complications and ensures consistent wound healing.
1. Patient Selection and Contraindications
Staplers are best suited for linear wounds with manageable tension and adequate soft tissue coverage. They are generally avoided in situations where closure conditions are suboptimal or cosmetic precision is critical.
Key considerations include:
- Thin or fragile skin: Areas over bone or critical structures may not tolerate staple placement well
- High-tension wounds: Increased risk of poor approximation or dehiscence
- Contaminated or infected wounds: May require alternative closure strategies
- Metal sensitivity: Consider alternatives in patients with known allergies
Staplers may be less appropriate in cosmetically sensitive areas or where wound edges are irregular. In such cases, suturing allows more precise control.
2. Proper Placement Technique
Once patient selection is appropriate, the stapler technique becomes the primary determinant of the quality of closure. Consistent positioning and spacing are essential for optimal results.
Key technique principles include:
- Accurate edge approximation: Ensure wound edges are aligned and slightly everted before firing
- Perpendicular device placement: Maintains proper staple formation
- Consistent spacing: Typically several millimeters between staples, depending on wound characteristics
- Visual inspection: Confirm proper staple formation before proceeding
Common technical errors include poor edge eversion, angling the device, and inconsistent spacing, all of which can affect wound healing and cosmetic outcomes.
3. Infection Prevention and Wound Care
Infection risk depends on multiple factors, including surgical technique, wound type, and patient condition. Adherence to sterile protocols remains essential regardless of closure method.
Best practices include:
- Strict aseptic technique: Use sterile devices and proper skin preparation
- Postoperative monitoring: Watch for erythema, drainage, or wound separation
- Appropriate removal timing: Based on anatomical location and healing progression
Evidence comparing infection rates between staples and sutures is mixed, with some studies showing differences and others reporting no significant variation.
4. Removal Best Practices
Proper removal technique is necessary to avoid additional tissue trauma and ensure patient comfort.
Key steps include:
- Use a dedicated staple remover: Deforms the staple for atraumatic extraction
- Assess wound healing before removal: Remove selectively if needed
Premature removal increases the risk of wound separation, while delayed removal may affect cosmetic outcomes.
5. Complication Recognition and Management
Although generally safe, stapled closures can be associated with complications that require early identification.
Potential complications include:
- Wound infection
- Dehiscence
- Staple loosening or displacement
- Visible scarring (“train-track” marks)
- Allergic reactions (rare)
Early signs such as increasing pain, redness, drainage, or wound separation should prompt reassessment and appropriate intervention.
Final Thoughts
Skin closure decisions extend beyond immediate approximation, influencing how efficiently procedures are completed and how consistently outcomes are achieved across cases.
As surgical volumes increase, the ability to standardize closure while reducing variability becomes an important part of overall workflow management.
In this context, subcuticular systems such as SubQ It! SU-25, designed for incisions up to 25 cm, offer an alternative approach for longer procedures. It enables dermal closure beneath the skin surface while removing the need for a separate staple removal step.
Contact our team to evaluate how SubQ It! SU-25 can simplify closure and reduce variability across cases.
FAQs
1. What is a skin stapler?
A skin stapler is a handheld surgical device used to close wounds by mechanically deploying staples that approximate the skin edges. It is widely used in operating rooms and emergency settings for rapid and consistent wound closure.
2. Is it painful to remove skin staples?
Most patients experience brief, mild discomfort during removal, typically described as a short pulling or pinching sensation. Proper technique using a dedicated staple remover minimizes tissue trauma.
3. Can you be allergic to surgical staples?
Allergic reactions are uncommon but can occur, most often related to nickel in stainless steel staples. In patients with known sensitivities, surgeons may consider titanium staples or bioabsorbable alternatives.
4. What material are skin staples made of?
Skin staples are commonly made from stainless steel or titanium, both of which are widely used due to their strength and biocompatibility. Bioabsorbable staples are made from synthetic polymers that gradually degrade and do not require removal.
5. Are surgical staples MRI safe?
Most modern skin staples are made from non-ferromagnetic materials and are considered MR Conditional, meaning they can be scanned safely under appropriate conditions. Patients should always inform imaging staff about any implanted materials.
6. How long should skin staples stay in before removal?
Removal timing depends on anatomical location and wound healing, typically ranging from about 7 to 10 days. The surgeon determines the timing based on the rate of healing, as early removal may increase the risk of dehiscence.
7. What are the advantages of using a skin stapler?
Skin staplers enable rapid and consistent wound closure, reducing operative time compared to suturing, particularly in longer incisions. They also simplify techniques and reduce variability between operators, supporting more efficient workflow in surgical settings.
8. What are the disposable skin stapler applications?
Disposable skin staplers are used to close linear surgical incisions in general surgery, orthopedics, obstetrics, and thoracic procedures. They are also widely used in emergency settings for laceration repair and trauma-related wound closure, where speed is critical.
Considering alternatives to traditional metal staples? SubQ It! offers bioabsorbable subcuticular staplers that deliver 7X faster closure than manual sutures while eliminating visible scarring and removal procedures. The FDA-cleared system places fasteners entirely subcutaneously, never piercing the external skin. Contact our team at +1 339-933-8811 or sales@subq-it.com to learn more about SubQ It! for your surgical practice.


