
Introduction
Choosing the right wound closure method directly affects surgical outcomes, patient comfort, and operating room efficiency. Often referred to as medical glue, medical skin adhesives offer a sterile, biocompatible alternative to sutures and staples, enabling quick and effective closure of wounds and surgical incisions.
Over the past two decades, the use of medical glue in modern surgery has grown significantly. It helps reduce closure time, minimize scarring, improve patient comfort, and eliminate the need for follow-up removal visits. Clinical studies) consistently show that tissue adhesives can save meaningful time compared to traditional suturing.
This blog breaks down what medical glue is, the key types available (cyanoacrylate-based and fibrin-based), their clinical applications, and how to select the right option for different surgical scenarios.
TL;DR
- Medical skin adhesives provide an effective alternative to sutures and staples for low‑tension, superficial wound closure, improving efficiency without compromising healing in many cases.
- Cyanoacrylate tissue adhesives are shown in randomized studies to produce comparable cosmetic outcomes and patient satisfaction to sutures, with faster and easier application.
- Evidence indicates adhesives can shorten closure time and may lower overall care burden, although prevention of dehiscence may still favor sutures in some contexts.
- Different adhesive types (e.g., cyanoacrylate vs. biological) serve distinct clinical applications, with cyanoacrylates most common for external skin closure.
- Selecting the right method depends on wound tension, location, and patient factors, ensuring adhesion is appropriate keeps outcomes optimal.
What Are Medical Skin Adhesives?
Medical skin adhesives are sterile, topical agents used to bond the edges of the skin together, enabling wound closure and healing by primary intention.
Typically formulated from cyanoacrylate compounds (such as 2-octyl or n-butyl cyanoacrylate), they polymerize on contact with moisture to form a thin, flexible barrier over the wound surface.
Breaking it down:
- Type: Topical wound-closure agent
- Formulation: Cyanoacrylate-based
- Function: Bonds skin edges and forms a protective film
- Application: External use on superficial skin wounds
How Medical Glue Works?
Medical skin adhesives polymerize (harden) upon contact with moisture on the skin surface, forming a thin, flexible film that holds wound edges in close approximation while healing occurs beneath.
Mechanism of Action:
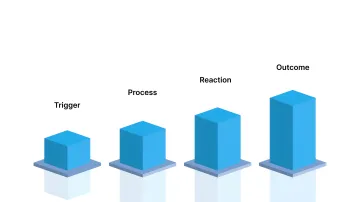
- Trigger: Contact with moisture (water, blood, or tissue fluids)
- Process: Cyanoacrylate monomers rapidly polymerize into long-chain molecules
- Reaction: Fast-curing reaction forming a stable, flexible polymer layer
- Outcome: Creates a secure adhesive film that holds wound edges together and maintains closure
What Makes Medical Skin Adhesives Effective for Wounds?
Surgical wound closure has relied on sutures and staples for decades, but these traditional methods create several challenges that impact both patient outcomes and healthcare efficiency.
Traditional closure methods often create problems:
- Suture marks leave permanent "train track" scarring along incision lines
- Staple removal causes significant patient discomfort and anxiety
- Materials passing through the skin increase infection risk by creating entry points for bacteria
- Follow-up appointments burden both patients and healthcare systems
Medical skin adhesives address these challenges for appropriate wound types:
- Comparable outcomes: Similar cosmetic results and wound healing in low-tension wounds vs sutures.
- Reduced procedure time: Faster application compared to conventional closure techniques.
- Barrier function: Forms a protective film that may help limit external contamination.
- Adjunct potential: Can be used alongside sutures to reinforce closure and protect the incision.
Recent evidence) indicates that cyanoacrylate-based adhesives can achieve comparable cosmetic outcomes and wound healing to sutures in superficial closures.
Why It Matters in Practice:
- Optimizes OR and ED efficiency without adding procedural complexity
- Expands closure options for surgeons in superficial, low-tension wounds
- Supports patient-centered care with less invasive techniques
- Aligns with modern wound management trends focused on speed, outcomes, and experience
Medical Skin Adhesives: Key Types and Clinical Applications
Medical skin adhesives exist in different chemical formulations, each designed for specific wound types, anatomical locations, and clinical scenarios. Understanding these differences helps surgeons optimize outcomes and avoid complications.
Cyanoacrylate-Based Adhesives
Cyanoacrylate adhesives are synthetic compounds (similar chemistry to "super glue" but medical-grade) that polymerize rapidly when exposed to moisture, forming a strong, waterproof bond. These are the most widely used medical skin adhesives, including products like Dermabond, Histoacryl, and LiquiBand.
These synthetic adhesives differ fundamentally from biological alternatives: they polymerize in seconds (fastest bonding time), create rigid waterproof seals, and work exclusively on external skin surfaces, not internal tissue.
This makes them ideal for:
- Low-tension lacerations and surgical incisions on the face, scalp, extremities, and torso
- Pediatric patients (eliminates needle anxiety and removal trauma)
- Emergency department wound closures where speed is critical
- Facial wounds requiring superior cosmetic outcomes
Cyanoacrylates offer several clinical advantages:
- Ultra-fast application (30-60 seconds total)
- Creates an immediate waterproof barrier (patients can shower after 24 hours)
- No removal required (sloughs off naturally in 7-10 days)
- Superior cosmetic results with no suture marks
- Antimicrobial properties that reduce infection risk
However, they have important limitations:
- Cannot be used on high-tension areas (joints, back, mechanically stressed regions)
- Not suitable for mucosal surfaces or constantly moist areas
- Can cause skin irritation in 2-5% of patients
- Should not be used on infected or contaminated wounds
- Limited flexibility once polymerized
Fibrin-Based Adhesives
Fibrin adhesives are biological sealants derived from human or animal blood proteins (fibrinogen and thrombin) that mimic the final stage of natural blood clotting. Products like TISSEEL and EVICEL create a soft, absorbable matrix that supports tissue healing.
Unlike synthetic cyanoacrylates, fibrin adhesives are biological, create flexible, absorbable seals, work through the natural clotting cascade, and excel in internal applications. Surgeons commonly use them for:
- Internal surgical applications (hemostasis during liver, spleen, or vascular surgery)
- Sealing air leaks in lung surgery
- Augmenting closure in friable or delicate tissues
- Patients with bleeding disorders requiring additional hemostatic support
Clinical benefits include:
- Biocompatible and biodegradable (fully absorbed by the body)
- Promotes natural healing processes
- Provides hemostatic effect (controls bleeding)
- Can be used on internal organs and tissues
- Flexible seal accommodates tissue movement
Their effectiveness is well-documented. In neurosurgery, Tisseel reduced postoperative CSF leaks from , demonstrating significant clinical value despite higher upfront costs.
How Do Surgeons Choose Skin Adhesives?
Selecting the appropriate medical skin adhesive requires systematic evaluation of multiple clinical factors. The "right" adhesive depends on wound characteristics, anatomical location, patient factors, and desired outcomes, not popularity or familiarity alone.
Wound Characteristics
- Tension Level:
- Low‑tension wounds: Topical cyanoacrylate adhesives are suitable for primary closure.
- High‑tension wounds: Mechanical closure (e.g., sutures or staples) is recommended because tissue adhesives alone do not provide sufficient tensile strength.
- Wound Depth:
- Superficial lacerations: Adhesives can usually be applied successfully.
- Deep or full‑thickness wounds: These typically require layered closure with sutures before a skin adhesive is applied to the superficial layer.
- Edge Quality:
- Clean, well‑approximated edges support optimal adhesive performance.
- Irregular or jagged edges generally require sutures for precise alignment before applying adhesive.
Anatomical Location
- Low‑movement, cosmetic areas: Cyanoacrylate adhesives are commonly used on the face, scalp, and other areas where cosmetic outcome and ease of use are priorities.
- High‑movement or mechanically stressed sites: Adhesives alone are typically inadequate on joints or other high‑tension regions, and sutures or staples are preferred.
- Moist or mucosal surfaces: Standard external skin adhesives are not indicated for constantly moist or mucosal areas, as bonding is unreliable and contraindicated in these applications.
Patient Factors
- Pediatric patients: Adhesives can reduce procedural pain and anxiety compared with sutures, especially in children and uncooperative patients.
- Patients with fragile skin: In older adults or those with fragile dermis, adhesives may minimize tissue trauma compared with repeated needle passes; however, clinical judgment is required to ensure adequate closure strength.
- Cosmetic concerns: While some studies show comparable cosmetic outcomes between adhesives and sutures in select low‑tension wounds, long‑term cosmetic advantages are not consistently superior and depend on wound location and closure technique.
For surgical incisions requiring both speed and cosmetic outcomes, bioabsorbable subcuticular closure systems like SubQ It! combine mechanical strength with absorption, eliminating the need for removal while providing faster closure than manual sutures.
Common Mistakes When Selecting Medical Skin Adhesives
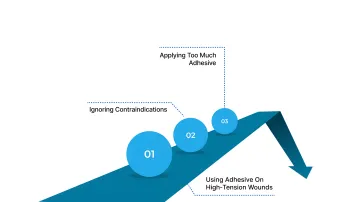
Choosing and applying medical skin adhesives requires clinical judgment and technique. Surgeons and clinicians can inadvertently compromise wound healing by overlooking key limitations and proper use parameters of cyanoacrylate‑based adhesives.
Using Adhesive on High‑Tension Wounds
One frequent error is applying cyanoacrylate tissue adhesive to wounds under significant mechanical stress (e.g., joints, back, or high‑movement areas). Standard cyanoacrylate adhesives are not intended for high‑tension closures; the pattern of failure is typically disruption at the skin–glue interface when excessive tension is present.
- Cyanoacrylate adhesives should be used only on low‑tension wounds or in combination with deep dermal sutures to offload tension before superficial closure.
- In high‑tension areas, sutures or staples remain the preferred mechanical closure method.
Ignoring Contraindications
Clinicians sometimes overlook established contraindications, which can lead to poor outcomes:
- Infected or heavily contaminated wounds: Adhesives are not recommended, as sealing over infection may hamper wound healing.
- Mucosal or constantly moist surfaces: Cyanoacrylate adhesives are designed for external skin use and do not bond reliably on moist tissues.
- Presence of ointments or contaminants: Surface residues (e.g., petroleum‑based ointments) can prevent proper adhesion.
- Known hypersensitivity: Allergic reactions to cyanoacrylate, formaldehyde, or related compounds can occur and should be screened for.
Applying Too Much Adhesive
Excessive adhesive application can create complications:
- Run‑off into the wound bed: Liquid adhesive may track into the wound, which can delay healing and cause irritation.
- Thick, rigid layers: Over‑application creates a bulky, stiff film that is more prone to cracking and failure under stress.
- Spread to surrounding skin: Unintended adhesive on intact skin can cause discomfort or require solvent removal.
Proper technique:
- Apply a thin, even layer of adhesive directly over well‑approximated skin edges. The goal is to form a discrete film that bonds the edges, not filling or pooling in the wound bed.
Final Thoughts
Medical skin adhesives have transformed modern wound management by offering faster closure and comparable cosmetic outcomes to traditional sutures in selected cases, particularly low‑tension, superficial wounds. Recent analyses of wound closure methods support that alternatives to conventional suturing can save operative time and enhance patient satisfaction without compromising healing quality.
For surgeons aiming to combine speed with predictability and improved cosmetic results, bioabsorbable subcuticular systems like SubQ It! have emerged as a compelling option. With each fastener deploying in about 7 seconds and closure achieved up to seven times faster than manual sutures, these systems eliminate the need for staple removal, reduce patient discomfort, and support minimal scarring.
Integrating SubQ IT! into your workflow can improve efficiency, minimize complications, and enhance patient outcomes. Contact the SubQ It! team to see how your practice can benefit.
FAQs
1. What exactly are medical skin adhesives, and how do they work?
Medical skin adhesives are sterile compounds (often cyanoacrylate‑based) that bond wound edges together by polymerizing on contact with moisture, forming a flexible film that approximates the skin while healing occurs beneath.
2. Are tissue adhesives as effective as sutures for wound closure?
In many low‑tension wounds, cyanoacrylate tissue adhesives have shown comparable cosmetic outcomes and patient satisfaction to sutures, while also being faster and easier to apply.
3. What types of tissue adhesives are used in clinical practice?
The main categories include cyanoacrylate adhesives (widely used for skin closure), fibrin‑based sealants (often for hemostasis or internal use), and protein‑based systems tailored for specific surgical contexts.
4. When should I avoid using medical skin adhesives?
Tissue adhesives are not recommended in high‑tension areas, moist or mucosal surfaces, or infected/contaminated wounds, as reliable adhesion and healing can be compromised.
5. Do tissue adhesives reduce pain and scarring compared to traditional methods?
Yes, because they eliminate sutures and needle passes, tissue adhesives often reduce pain, anxiety, and visible marks, especially in pediatric and cosmetic cases.
6. How much time do tissue adhesives save vs. sutures?
Cyanoacrylate adhesives polymerize quickly and can shorten closure time significantly compared to sutures in many settings, making them efficient for routine superficial closures.
7. Are there risks or complications with medical skin adhesives?
While tissue adhesives are generally safe, inappropriate use (e.g., too much adhesive, improper wound selection) can lead to inflammation, delayed healing, or adhesive failure at the wound interface.


