Abdominal wound closure decisions in open abdomen cases arise when primary fascial closure is not feasible. In these situations, the selected device determines how the abdomen is stabilized and whether delayed closure remains achievable.
The importance of this decision is reflected in market projections, which expect abdominal closure technologies to reach USD 273.33 million by 2036.
This growth parallels an increasing clinical reliance on systems that influence fluid control, fascial preservation, and the risk of complications.
In this blog, you’ll explore how abdominal wound closure devices are used in 2026 and how surgeons select the appropriate approach based on patient condition and closure goals.
Key Takeaways:
- Abdominal wound closure devices are used when primary fascial closure is not safe, helping stabilize the abdomen and allow planned re-entry.
- Each device type serves a specific purpose, including fluid control, fascial alignment, or temporary coverage, and they are not interchangeable.
- Negative pressure systems help manage fluid and protect tissue, but require traction support to prevent fascial edges from separating.
- Achieving delayed primary fascial closure depends on early decisions, with outcomes declining if closure is delayed beyond 5-7 days.
- Device selection should adapt to patient condition, contamination, and closure goals, rather than relying on a single approach throughout treatment.
What Is an Abdominal Wound Closure Device in Open Abdomen Management?
In open-abdomen management, an abdominal wound-closure device is used when primary fascial closure is not clinically safe. After laparotomy, the fascia is intentionally left open to avoid complications such as abdominal compartment syndrome.
At this stage, the abdomen requires controlled temporary coverage rather than definitive closure. The selected device determines whether delayed primary fascial closure remains achievable. It also influences the risk of complications such as fascial retraction or ventral hernia.
These devices are not functionally interchangeable. Each device manages the open abdomen differently:
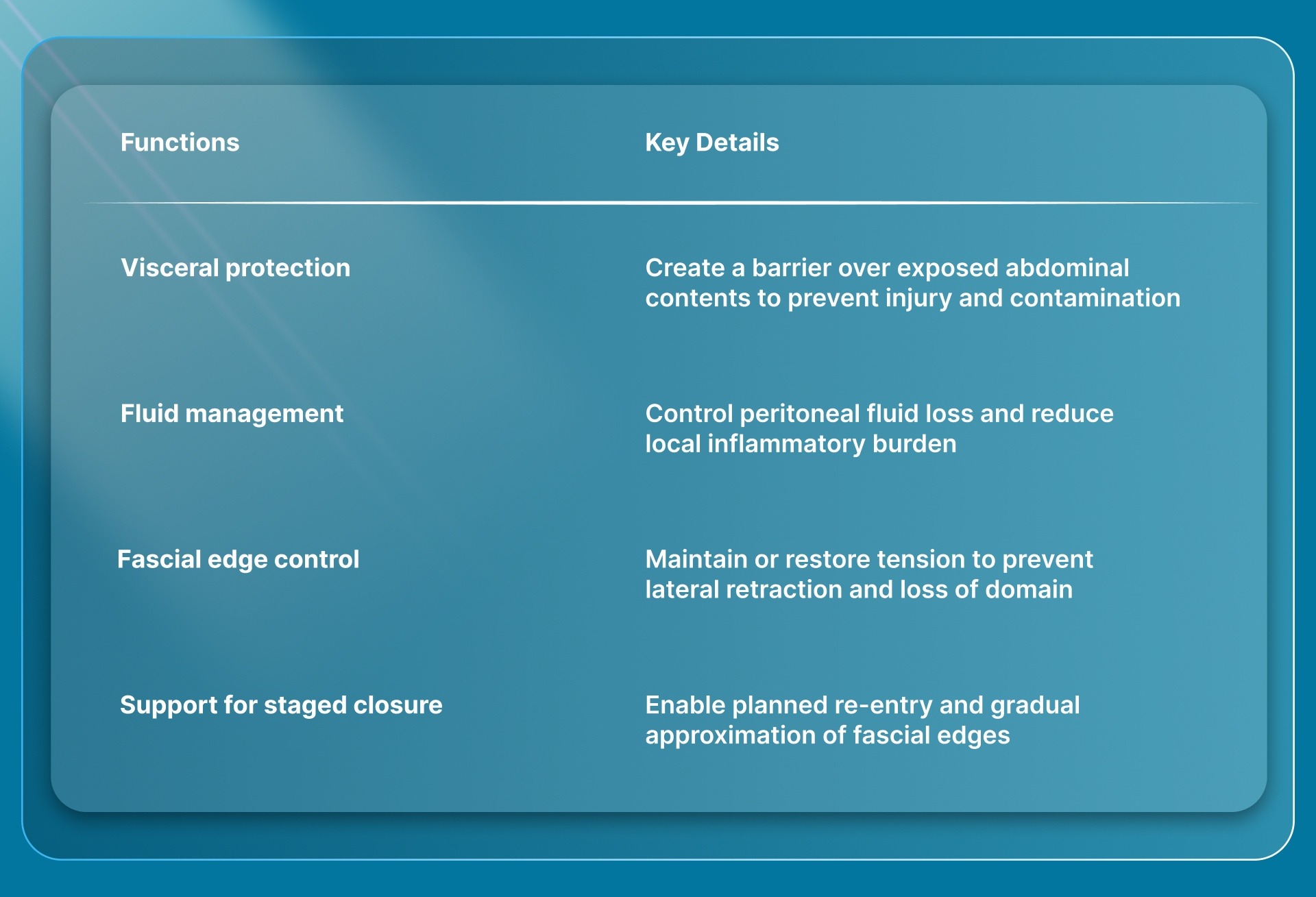

A clear understanding of the device also helps explain the situations in which surgeons choose to use it.
When Do Surgeons Use Abdominal Wound Closure Devices?
Abdominal wound closure devices are used when immediate fascial closure is not clinically safe or would increase the risk of complications. This decision typically follows a damage-control laparotomy, in which physiologic instability takes priority over definitive closure.
The following clinical scenarios guide when these devices are used:

In these scenarios, the closure device becomes part of a staged surgical approach. It supports physiologic recovery while preserving the ability to achieve delayed primary fascial closure.
Closing longer incisions at the skin level may benefit from bioabsorbable subcuticular systems such as SubQ It! SU-25, which places absorbable fasteners beneath the skin surface and eliminates the need for removal.
Once the clinical indications are clear, it becomes important to review the main device types.
5 Types of Abdominal Wound Closure Devices
Abdominal wound closure devices used in open abdomen management differ in how they protect viscera, manage fluid, and control fascial edges.
Each category serves a specific role, and selection depends on the clinical goal, the timeline to closure, and the patient's condition.
The following categories represent the primary abdominal wound closure devices used in practice:
1. Negative Pressure Wound Therapy (NPWT) Devices
NPWT devices use a foam or gauze interface placed over the viscera, sealed with an occlusive dressing, and connected to a controlled suction device.
- Primary function: Fluid removal and visceral protection
- Mechanism: Applies continuous negative pressure to evacuate peritoneal fluid and reduce edema
- Clinical role: Commonly used as a baseline approach in open abdomen management
- Limitation: Does not provide active fascial traction, allowing lateral retraction over time
2. Dynamic Fascial Traction Devices
These devices apply continuous or adjustable tension to fascial edges to prevent retraction and support delayed closure.
- Primary function: Maintain or restore fascial edge alignment
- Mechanism: Mechanical traction applied through sutured or external systems
- Clinical role: Used when early primary fascial closure is the goal
- Consideration: May require repeated adjustments or additional operative time
3. Mesh-Based Closure Devices
Mesh devices are used when fascial edges cannot be approximated despite traction and require bridging.
- Primary function: Structural support and domain preservation
- Types: Biologic and synthetic mesh
- Clinical role: Used when primary fascial closure is not achievable
- Limitation: Often results in a planned ventral hernia requiring later reconstruction
4. Temporary Barrier Devices (Plastic Silo / Bogotá Bag)
These are simple barrier systems made of sterile plastic to cover the open abdomen.
- Primary function: Immediate visceral protection
- Mechanism: Physical barrier without fluid control or traction
- Clinical role: Used in emergency or resource-limited settings
- Limitation: Higher risk of fluid loss, infection, and fascial retraction
5. Skin Approximation Devices
These devices approximate the skin layer without closing the fascia, providing temporary coverage.
- Primary function: Protect abdominal contents and reduce fluid exposure
- Methods: Towel clips, running sutures, or zipper systems
- Clinical role: Used when fascial closure is not achievable in the short term
- Limitation: Does not support fascial closure and carries a higher complication risk
Once the available options are clear, the next consideration is how to select the most appropriate device for the situation.
How to Choose the Right Abdominal Wound Closure Device?
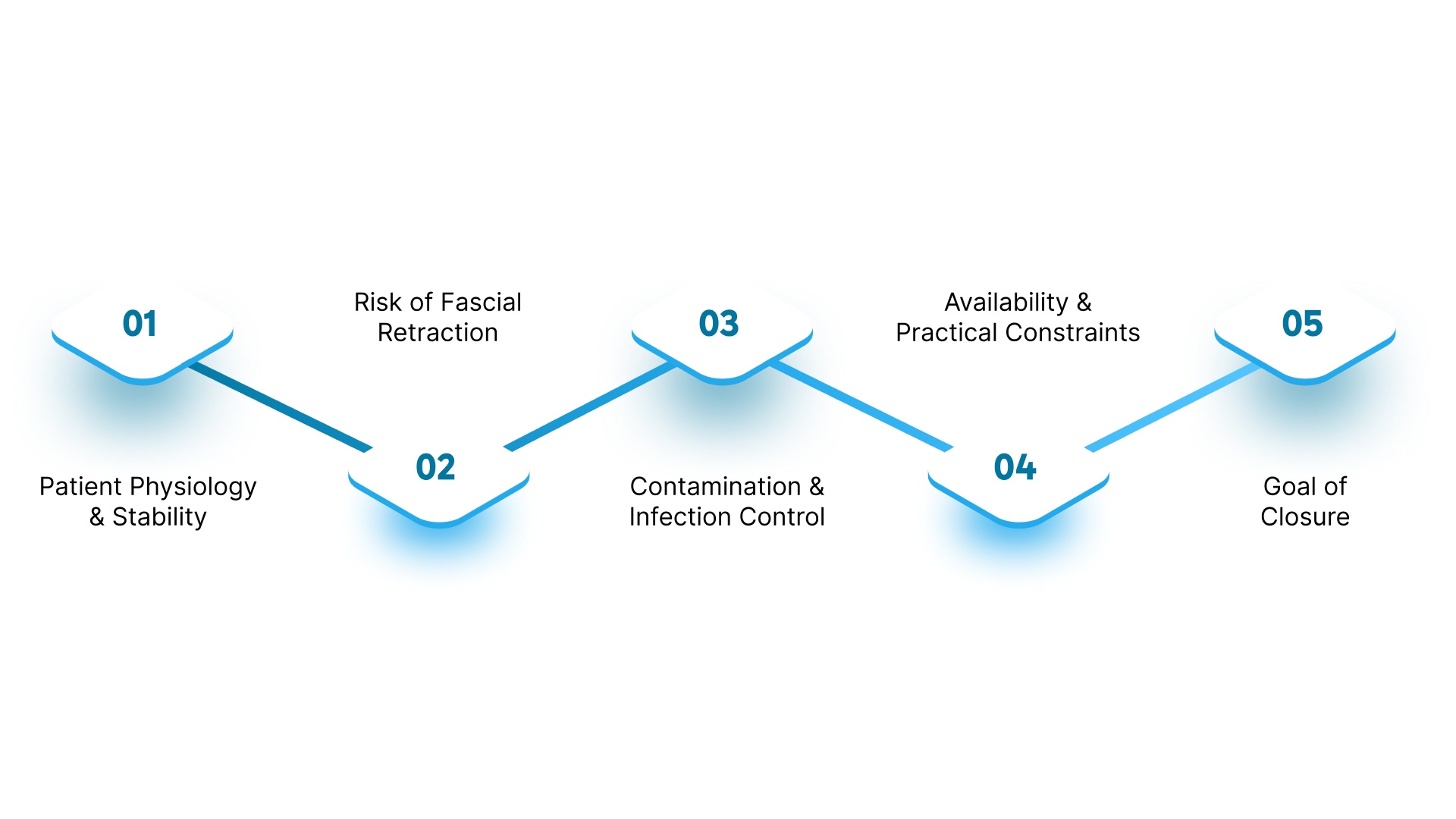
Choosing an abdominal wound closure device depends on whether delayed primary fascial closure is achievable and how quickly it needs to be achieved. The decision is driven by patient physiology, contamination, and the expected timeline to closure.
Device selection should prioritize fascial preservation, fluid control, and progression toward delayed primary fascial closure. The following factors guide selection in practice:
1. Patient Physiology and Stability
Physiologic status determines how much intervention the patient can tolerate during the initial operation and subsequent re-entries. In unstable patients, the priority shifts from closure to rapid control and recovery.
This directly influences how aggressively closure strategies can be applied:
- Unstable physiology (acidosis, hypothermia, coagulopathy): Use rapid, low-complexity options such as NPWT or barrier systems to minimize operative time and support stabilization
- Stabilizing patients: Introduce traction-based devices early to prevent fascial retraction and preserve closure potential
- Severely compromised patients: Avoid techniques that require prolonged operative time or repeated adjustments during early resuscitation
2. Risk of Fascial Retraction
Fascial retraction begins early and can quickly limit the ability to achieve delayed closure. Preventing loss of domain is a key objective during open abdomen management.
Device choice should reflect the expected risk of retraction:
- Early phase with low retraction risk: NPWT alone may provide temporary control without immediate traction
- Moderate to high risk of retraction: Use traction devices to maintain fascial alignment and prevent lateral migration
- Delayed cases (5–7 days): Traction becomes critical, as closure probability declines without active tension
3. Contamination and Infection Control
The intra-abdominal environment affects both device selection and timing of closure strategies. Contamination requires a balance between fluid control and preservation of closure potential.
Device strategy should adapt as contamination is addressed:
- Contaminated abdomen: NPWT supports fluid evacuation and helps manage the inflammatory burden during source control
- Ongoing infection: Avoid premature use of bridging strategies unless fascial closure is not achievable
- After source control: Transition toward traction-based systems to support progression to closure
4. Availability and Practical Constraints
Device selection is influenced by access, expertise, and operative workflow considerations. These factors affect what can be implemented safely and consistently.
Practical constraints should be considered alongside clinical goals:
- Access to traction systems: Enables more effective prevention of fascial retraction and higher closure success
- Limited resources: Barrier methods may be used initially for rapid coverage in emergency settings
- Operative workload and follow-up: Devices requiring fewer adjustments may be preferred in high-demand environments
5. Goal of Closure
Defining the intended outcome early helps guide device selection and avoid delays in escalation. The approach differs depending on whether closure is achievable.
The chosen strategy should align with the end goal:
- Primary fascial closure: Use traction-based systems early to maximize closure probability
- Delayed closure with preservation: Combine fluid control and fascial management to maintain closure potential
- Planned hernia approach: Use bridging strategies when fascial closure is not achievable despite intervention
While choosing the right device is essential, recognizing frequent selection pitfalls is equally important.
Common Mistakes in Abdominal Wound Closure Device Selection
Abdominal wound closure device selection directly affects whether delayed primary fascial closure remains achievable. Most complications arise from how the closure strategy evolves over time rather than the initial decision.
Avoiding the following mistakes can significantly improve closure outcomes and reduce long-term complications:

Final thoughts
Abdominal wound closure in open abdomen cases extends beyond achieving fascial approximation. It continues to influence recovery consistency, follow-up requirements, and the predictability of outcomes across procedures.
As expectations for efficient closure and controlled healing increase, the role of skin closure becomes more relevant in the overall closure pathway.
In this context, SubQ It! SU-25 provides a bioabsorbable subcutaneous closure system designed for longer incisions, with 25 staples supporting closure up to 25 cm. The system places absorbable fasteners beneath the skin to approximate wound edges without external penetration.
Because the fasteners are bioabsorbable and placed subcutaneously, there is no need for a follow-up visit for staple removal, while also saving approximately 25 minutes per case.
Contact us to explore how SubQ It! SU-25 fits into your closure workflow, and learn more about its clinical application.
FAQs
1. What is the difference between temporary abdominal closure and an open abdomen?
An open abdomen refers to a condition in which the fascia is intentionally left open after surgery. Temporary abdominal closure describes the method used to protect and manage the abdominal contents during this period until closure becomes feasible.
2. Can abdominal wound closure devices affect ICU or hospital stay?
Device choice can influence fluid control and physiologic stabilization, which in turn affects the timing of definitive closure. While outcomes vary, this may impact overall recovery progression and length of stay.
3. Can different abdominal wound closure devices be used together during treatment?
Yes, combination approaches are commonly used. For example, negative pressure systems are often combined with fascial traction to support both fluid control and preservation of fascial alignment during staged closure.
4. Do all open abdomen cases result in primary fascial closure?
Not all cases achieve primary closure. Delays, tissue condition, and prolonged open abdomen duration can reduce the ability to approximate fascial edges later.
5. Why is intra-abdominal pressure important during closure decisions?
Intra-abdominal pressure helps determine whether the abdomen can be safely closed. Elevated pressure increases the risk of abdominal compartment syndrome, which can compromise organ function if closure is attempted prematurely.
6. Are abdominal wound closure devices single-use or reusable?
Most modern systems are designed for single use to maintain sterility and consistent performance. The choice may vary depending on the device type and its use in the surgical workflow.