A plastic surgeon finishes a case, reaches for a disposable stapler, and closes in under two minutes. Ten days later, the patient comes back for staple removal with visible puncture marks along the incision line.
The speed and outcome trade-off also shows up in the data. A 2025 database analysis of 18,268 leg bypass procedures found that metal staple closure was linked to 57% higher chances of SSI compared to sutures. Speed matters, but it shouldn't be the only factor in your closure decision.
This post covers the Everready First Aid disposable skin stapler and breaks down where bioabsorbable alternatives fit into a modern surgical practice.
Key Takeaways
- The Everready First Aid disposable skin stapler is a single-use device preloaded with 35 wide staples (6.5 mm x 4.7 mm) and bundled with a sterile remover.
- Scar satisfaction scores in thyroid surgery and cesarean studies consistently favor under-the-skin sutures over surface metal staples.
- Every metal staple closure requires a follow-up removal visit, adding scheduling burden and patient discomfort.
- Infection risk evidence is procedure-specific, and metal staples may still be reasonable in settings where speed is the top priority.
- Bioabsorbable under-the-skin closure systems now offer stapler-level speed without surface puncture marks or removal visits.
What is the Everready First Aid Sterile Disposable Surgical Skin Stapler?
The Everready First Aid sterile disposable surgical skin stapler is a single-use metal skin closure device made by Ever Ready First Aid. It comes preloaded with 35 wide staples measuring 6.5 mm x 4.7 mm and ships with a sterile staple remover in the same package.
This device is sold primarily through EMS supply retailers and online marketplaces. It's designed for external skin closure, meaning the metal staples sit on the surface of the skin and hold wound edges together until they're removed at a follow-up visit, typically 7 to 10 days after surgery.
For surgeons in private practice or ambulatory surgical centers, it's worth knowing where this device fits among today's skin closure options, and what tradeoffs come with choosing it.
How Does the Everready First Aid Skin Stapler Work?
The Everready stapler works like most disposable metal skin staplers. You position the device over the wound edges, squeeze the handle, and a single staple fires through both sides of the skin to hold the incision closed. Each squeeze advances the next staple automatically.
Here's what the basic workflow looks like in practice.
- Wound preparation: Clean and align the wound edges so they sit evenly before stapling. Skin tension should be minimal at the closure site.
- Staple placement: Position the stapler perpendicular to the incision line, press the device gently against the skin, and squeeze the handle to fire. Space each staple evenly along the incision.
- Post-closure check: Confirm that each staple sits flat against the skin surface, and that wound edges are well-approximated (evenly aligned) without gaps or overlapping tissue.
- Scheduled removal: Metal staples require a follow-up visit for removal using the included staple remover. Timing depends on the anatomical site and healing progress.
The device is single-use and non-reloadable. Once all staples are fired, the stapler is discarded.
One thing to note is that because the staples sit on the outer skin surface, they create small percutaneous puncture points on both sides of the incision. These are the entry and exit marks that can leave railroad-track scars after removal, which is one of the key tradeoffs surgeons weigh when choosing between staples and sutures.
Is the Everready First Aid Skin Stapler Worth It?
For some procedures, a disposable metal stapler like the Everready model is a reasonable, practical choice. For others, the tradeoffs in infection risk, scarring, and follow-up visits work against both the surgeon and the patient.
Infection Risk
The infection risk from staples varies by procedure type. In vascular and orthopedic cases, the data favoring sutures is stronger. In abdominal surgery, the difference is less clear.
Scarring
A 2025 study on 100 thyroid surgery patients found that staplers closed faster, but patients rated their scars worse compared to the suture group. The study used the Patient and Observer Scar Assessment Scale (POSAS), a standard tool for measuring scar satisfaction.
Metal staples leave small puncture marks on both sides of the incision, often called railroad-track scars. For scheduled and cosmetic cases, this is one of the most common patient complaints after staple removal.
Removal Visits
Every metal staple closure requires a follow-up visit for removal. That adds staff time, scheduling work, and patient inconvenience. For practices with high case volume, the time spent on removal visits adds up quickly over a month.
Cost of Complications
Individual wound infections cost between $5,600 and $12,900 per case. According to data, wound infections cost the healthcare system roughly $3.3 billion annually overall. A cheap stapler that raises infection risk even slightly can become the most expensive option over time.
For surgeons in planned (non-emergency) settings where scar quality and patient satisfaction matter, the tradeoffs with metal disposable skin staplers are worth weighing carefully.
What are Bioabsorbable Alternatives to Metal Skin Staplers?
Bioabsorbable subcuticular skin closure systems place dissolving fasteners under the skin surface instead of through it. The fasteners hold the wound edges together during healing and are absorbed by the body, typically over 90 to 120 days. No removal visit is needed.
A study of 4,311 mastectomy patients compared an absorbable subcuticular stapler to hand-sewn sutures. The absorbable stapler group had higher baseline risk factors (older age, higher rates of diabetes and hypertension), yet SSI rates were comparable. The absorbable stapler also significantly reduced skin closure time.
A study from the University of Pennsylvania evaluated an absorbable dermal stapler during panniculectomy (removal of excess abdominal tissue). The absorbable stapler reduced operative time without compromising outcomes, consistent with earlier data showing absorbable devices can close at up to seven times the speed of hand suturing.
For surgeons closing incisions, the tradeoff between speed and cosmetic outcome is a recurring frustration. Metal staplers save time but leave surface marks and require removal. Hand suturing gives better cosmesis but takes significantly longer.
Bioabsorbable subcuticular systems close that time difference. SubQ It! delivers closure at roughly seven times the speed of hand suturing. For the SubQ It! SU-25 variant (25 fasteners, incisions up to 25 cm), that translates to approximately 25 minutes saved per case compared to manual subcuticular skin closure. In a private clinic, 25 minutes saved can mean one additional patient per day, roughly $6,000 in additional revenue.
If you're currently using a disposable metal skin stapler and your patients care about scar appearance, or if removal visits are a scheduling burden, bioabsorbable subcuticular closure is worth evaluating.
How Do Metal Staplers and Bioabsorbable Systems Differ in Practice?
The sticker price on a disposable metal skin stapler is low. That looks inexpensive until you account for what happens after the procedure. Here's a side-by-side look at the practical differences between metal staplers and bioabsorbable subcuticular systems.
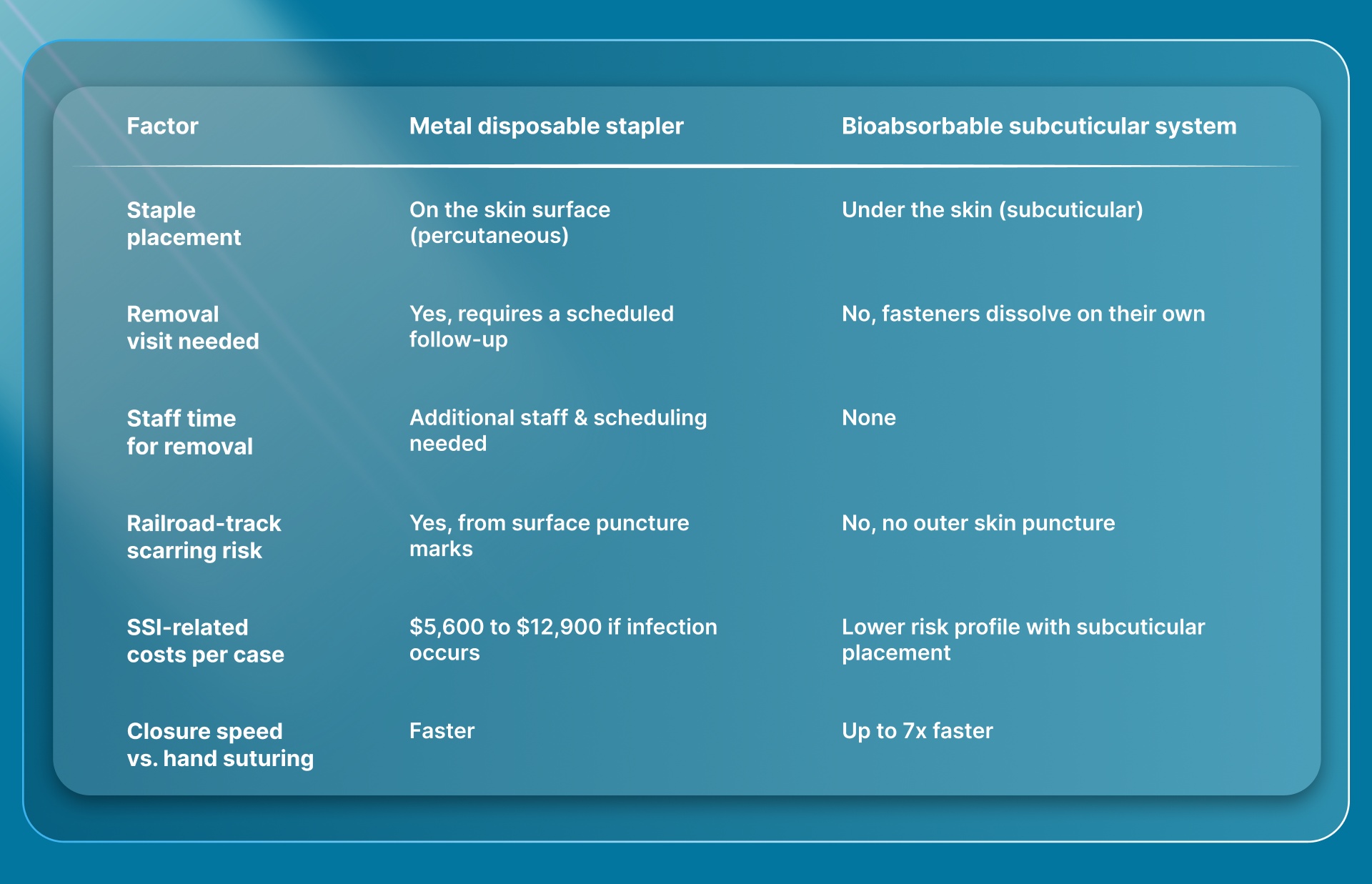

Metal staplers are fast. Most studies confirm closure times under 5 minutes for typical incisions. Subcuticular hand suturing takes longer, sometimes 20 to 25 minutes for a moderate-length incision.
When are Disposable Metal Skin Staplers Still Appropriate?
Metal staplers aren't always the wrong choice. Clinical context matters, and there are situations where a disposable metal skin stapler is still a reasonable option. Here are the scenarios where metal staplers continue to make clinical sense.
- Trauma and emergency settings: When speed is the priority and cosmetic outcome is secondary, a fast metal stapler can save critical minutes.
- Scalp closures: The scalp has a rich blood supply and hair coverage, making cosmetic concerns and SSI risk lower than in other anatomical areas.
- High-risk anesthesia patients: For patients where every minute under anesthesia increases risk, the fastest closure method may be the safest overall choice.
- Field and pre-hospital care: In EMS and wilderness medicine contexts, a preloaded disposable stapler like the Everready model is practical and portable.
The key is matching the device to the clinical scenario. A surgical skin stapler designed for field use or emergency departments serves a different purpose than a closure system designed for elective procedures in a private practice OR. Choosing the right tool for the right case is what separates a good outcome from a preventable complication.
For cases where cosmetic results, patient satisfaction, and total cost of care matter, the evidence increasingly supports subcuticular closure over surface metal staples. For urgent cases where seconds count, a disposable stapler still earns its place on the tray.
Final Thoughts
Disposable metal skin staplers like the Everready First Aid model are widely available, affordable, and fast. Those are real advantages. The tradeoffs, including SSI risk in certain procedures, railroad-track scarring, and mandatory removal visits, are equally real.
If you're evaluating skin closure devices for an elective surgical practice, look beyond unit cost. Consider the full picture of infection risk, cosmetic outcome, patient experience, and follow-up burden. The right closure method should serve your patients and your practice at the same time.
SubQ It! gives surgeons a bioabsorbable subcuticular option that matches stapler speed without surface punctures or removal visits. Whether you're running a high-volume laparoscopic practice or a cosmetic surgery center, it's worth seeing how bioabsorbable closure fits your workflow. Contact us today to request a custom quote and learn how SubQ It! can work for your cases.
FAQs
1. How Many Staples Does a Typical Disposable Skin Stapler Hold?
Most disposable skin staplers come preloaded with enough staples to close a single incision, though the exact count varies by model and manufacturer. The staple count determines how long an incision you can close with a single device.
2. How Long Do Metal Skin Staples Stay in Before Removal?
Yes, metal skin staples need to be removed within roughly one to two weeks post-op, depending on the incision site. A separate staple remover tool is used during a follow-up office visit.
3. Can Disposable Skin Staplers Be Used on Any Body Part?
No, disposable skin staplers are best suited for areas with enough tissue thickness to support a metal staple. They're commonly used on the scalp, torso, and extremities but avoided on the face and delicate skin.
4. Do Metal Skin Staples Always Leave Visible Scars?
Yes, metal staples placed through the skin surface often leave small puncture marks on both sides of the incision line. These marks are sometimes called railroad-track scars and are more visible on certain skin types.
5. What Is the Difference Between a Reusable and Disposable Skin Stapler?
Reusable skin staplers are designed for sterilization and repeated use across patients, while disposable models are single-use and discarded after one procedure. Disposable models reduce cross-contamination risk.
6. Are Skin Staplers Faster Than Hand Suturing?
Yes, skin staplers consistently close wounds faster than hand suturing. Most stapler closures finish in a few minutes, while subcuticular hand suturing on moderate incisions takes considerably longer.


