Suture devices remain central to surgical wound closure, yet the final phase can significantly affect operative time and workflow, depending largely on the chosen closure method.
Manual suturing offers control but requires repeated needle passes and knot tying, making duration dependent on incision length and technique.
On the other hand, staples can reduce closure time by up to 80%, with comparable cosmetic outcomes in appropriate cases.
In this blog, you’ll explore how surgeons evaluate suture devices in 2026, including performance criteria, clinical limitations, and their impact on procedural workflow.
Key Takeaways:
- Suture devices are used to approximate tissue across the skin, subcutaneous, and fascial layers, providing control and flexibility in closure.
- Manual suturing is time-intensive and technique-dependent, especially in longer or multi-layer incisions.
- Alternative closure methods, including device-assisted systems, are used where speed and standardization are priorities, especially in high-volume or repetitive procedures.
- Closure time directly affects operating room efficiency, including case duration, turnover, and scheduling predictability.
- Evaluating a suture device involves assessing tissue compatibility, handling, closure time, and overall procedural fit.
What Is a Suture Device?
A suture device refers to a system or instrument used to place sutures for tissue approximation and wound closure during healing. It may include a needle with attached suture material or a device that assists in delivering and securing sutures.
The needle passes through tissue layers, allowing the suture to approximate wound edges under controlled tension. This is used to close skin, subcutaneous tissue, and deeper structures such as fascia.
Selection depends on tissue characteristics, incision depth, and required tensile strength, as these factors directly influence tissue approximation, stability, and healing outcomes.
These selection considerations are reflected in comparative clinical outcomes observed across different closure methods.
Real Case Study
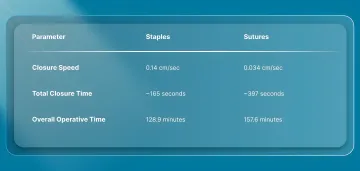
A comparative clinical study evaluating skin staples versus sutures for midline abdominal wound closure demonstrated measurable differences in closure efficiency and operative time.
- Closure speed was higher with staples (0.14 cm per second) compared to sutures (0.034 cm per second)
- Total closure time was shorter in the staple group (approximately 165 seconds) compared to sutures (approximately 397 seconds)
- Overall operative time was reduced when staples were used (128.9 minutes vs 157.6 minutes)
Despite faster closure:
- No significant difference was observed in surgical site infection rates between staples and sutures
- Cosmetic outcomes were reported as comparable between the two methods
These findings indicate that mechanical closure methods can reduce closure time without compromising safety or cosmetic outcomes, particularly in procedures where efficiency and consistency are important.
After defining what a suture device is, it becomes easier to understand the primary types used in clinical practice.
3 Key Types of Suture Devices

Suture devices used in surgical closure can be grouped based on how sutures are placed, secured, and managed during a procedure. Each type affects closure time, consistency, and control differently.
1. Manual Suturing Systems
Manual suturing involves a needle and suture thread, which is placed and secured by hand.
- Allows precise control over needle placement and tension
- Common techniques include interrupted and continuous suturing
- Used across the skin, subcutaneous tissue, and deeper layers, such as fascia
2. Barbed Suture Systems (Knotless Sutures)
Barbed sutures incorporate small projections along the thread that anchor into tissue.
- Eliminate the need for knot tying
- Distribute tension evenly along the wound
- Used in soft tissue and fascial closure, including minimally invasive procedures
3. Preloaded Suture Systems
These consist of needles pre-attached to suture material in standardized configurations.
- Reduce preparation and handling time
- Ensure consistent needle-suture combinations
- Widely used across surgical procedures for efficiency and reliability
While these systems remain widely used, closure approaches are not limited to sutures alone.
In procedures involving longer incisions, device-assisted systems such as SubQ It! SU-25, designed to close incisions up to 25 cm, offers an alternative approach by placing bioabsorbable fasteners beneath the skin.
It reduces closure time and supports a more consistent workflow in high-volume or time-sensitive settings.
Once the types are clear, their practical use across surgical specialties becomes the next important consideration.
4 Use Cases of Suture Devices by Surgical Specialty
Suture devices are used across surgical procedures for tissue approximation, particularly where controlled closure, layered repair, or mechanical stability is required.
1. Abdominal Surgery
In abdominal procedures, sutures are primarily used for fascial closure, where strength and durability are critical.
- Suitable for midline and deep fascial layers
- Allow controlled tension across longer incisions
- Common in procedures requiring multi-layer closure
2. Gynecologic and Obstetric Procedures
In procedures such as cesarean sections, sutures are used for layered closure across multiple tissue types.
- Applied to the uterine and fascial layers
- Support structured, stepwise closure
- Selected based on the healing requirements of each layer
3. Plastic and Reconstructive Surgery
Sutures are used where precise edge alignment is required, especially in visible areas.
- Enable controlled subcuticular and fine closure techniques
- Used in procedures where scar appearance is a key consideration
4. Orthopedic Surgery
Orthopedic procedures involve high-tension closures, particularly around joints and load-bearing areas.
- Used for deep tissue and fascial approximation
- Maintain closure under mechanical stress and movement
- Common in joint replacement and trauma procedures
Beyond their clinical applications, it is also important to understand how suture devices influence closure time and overall operating room efficiency.
How Suture Devices Impact Closure Time & OR Efficiency?
Suture devices directly influence closure duration and variability at the final stage of a procedure.
Although closure occurs at the end of the operating room workflow, it has a measurable impact on total operative time, turnover, and scheduling predictability.
1. Closure Time with Manual Suturing
With traditional suture devices, closure is performed step by step:
- Needle placement through tissue
- Suture pull-through
- Tension adjustment
- Knot tying
This sequence is repeated along the length of the incision.
- In shorter incisions, the time impact is limited
- In longer or multi-layer closures, closure time increases proportionally
- Precision-driven techniques further extend the closure phase
2. Technique Dependency and Variability
Closure time with sutures varies based on:
- Technique used (interrupted vs continuous)
- Tissue type and tension
- Length of the incision
- Individual handling and consistency
This introduces variability between cases, even for similar procedures.
From an operational standpoint, this affects:
- Case scheduling
- Turnover between procedures
- Overall Operating Room (OR) utilization
3. Impact on OR Workflow
Because closure occurs at the end of the procedure, delays at this stage affect:
- Total time in the operating room
- Transition to the next case
- Staff and resource allocation
In high-volume settings, even small increases in closure time per case accumulate across multiple procedures.
Their effect on operating room performance makes it essential to assess how a suture device should be evaluated for surgical use.
How to Evaluate a Suture Device for Surgical Use?
Evaluating a suture device requires assessing its mechanical performance, handling, and its impact on the procedural workflow. The key question is how the device performs during closure and how consistently it supports outcomes across cases.
1. Match the Device to Tissue and Tension Requirements
Different procedures place different mechanical demands on closure.
- High-tension areas such as fascia or joint-adjacent tissue require strong, durable support
- Lower-tension areas, such as superficial skin, allow for finer, more precise closure
The device should maintain adequate strength during the initial healing phase without compromising tissue integrity.
2. Assess Closure Time Per Case
Closure time is a practical factor in device evaluation.
- Manual suturing involves repeated needle passes and knot tying
- Time increases with incision length and the number of layers
When evaluating a suture device, consider:
- Time required to complete closure
- Consistency of closure time across similar procedures
- Impact on overall case duration
3. Evaluate Technique Dependency
Suture-based closure is technique-sensitive.
- Needle angle, spacing, and tension vary with handling
- Outcomes can differ across cases depending on the technique
A device should allow predictable placement and consistent approximation, especially in frequently performed procedures.
4. Review Handling and Ergonomics
Ease of use affects both precision and efficiency.
- Needle control during placement
- Visibility in the operative field
- Comfort during repeated use
Difficult handling can increase closure time and affect consistency.
5. Consider Fit Within the Procedure
Not all suture devices are suited to every use case.
- Layered closures may require multiple techniques
- Minimally invasive procedures require adapted access and instrumentation
- Longer incisions increase the time burden of manual closure
Evaluation should focus on how well the device fits the procedural workflow.
6. Account for Post-Operative Implications
The choice of closure method affects post-operative outcomes.
- Whether follow-up intervention is required (e.g., removal in non-absorbable systems)
- Stability of the wound during early healing
- Tissue response, infection risk, and cosmetic outcome
These factors influence both patient recovery and practice workflow.
Final Thoughts
Closure with suture devices does not end at tissue approximation. It continues to influence operative time, consistency of closure across cases, and post-operative workflow.
As procedural demands increase, the limitations of manual, technique-dependent closure become more visible in both time and consistency.
In this context, systems like SubQ It! SU-25 represents a subcutaneous, device-assisted approach for longer incisions, placing bioabsorbable fasteners beneath the skin surface without external penetration. They help reduce variability in closure time.
Contact us to explore how SubQ It! SU-25 fits into your surgical workflow and evaluates its role in improving closure efficiency.
FAQs
1. What is a suture device?
A suture is a needle-and-thread device used to approximate tissue during wound closure. In addition to sutures, mechanical closure systems use fasteners to approximate tissue.
2. What are the three suturing instruments?
The three essential instruments are:
- Needle holders to control the needle
- Tissue forceps to handle tissue
- Suture scissors to cut the thread
3. How do bioabsorbable sutures compare to traditional sutures?
Bioabsorbable sutures degrade over time and do not require removal. Non-absorbable sutures require removal or remain permanently, depending on use.
4. What are the advantages of automated suturing devices?
Automated closure devices reduce the time required for skin closure and provide a standardized technique. They improve placement consistency, particularly in procedures where closure speed and reproducibility are important.
5. How long does wound closure take with advanced suturing devices?
Closure time varies depending on incision length, technique, and surgical setting. Mechanical systems are generally faster than manual suturing, but the exact time difference depends on procedural and operator factors.
6. What should hospitals consider when evaluating suturing devices?
When evaluating suturing devices, hospitals should consider:
- Regulatory clearance for intended use
- Clinical evidence supporting performance
- Ease of integration into the surgical workflow
- Training requirements and learning curve
- Impact on post-operative management and follow-up
- Total cost of care across the procedure