
A needle for stitches carries the suture through tissue, and the point shape decides how clean that pass occurs. Taper, cutting, and reverse cutting all behave differently in skin. A mismatch means more tearing and a rougher scar at follow-up.
Taper points needed 4.07 N of force to tear through tissue in recent testing, compared to 3.26 N for conventional cutting needles. On delicate tissue, that difference is visible when the patient comes back.
This post covers needle point types, curvature, and how to read suture pack codes. It also covers when skipping the needle for skin closure is the faster and cleaner option.
Key Takeaways
- A needle for stitches has three working zones that shape how it moves through tissue: the point, the body, and the swage.
- Taper points pierce and spread tissue and are the standard for bowel, vessels, fascia, and subcutaneous closure.
- Reverse-cutting needles are preferred for skin because the outer cutting edge reduces pull-through at the wound edge under tension.
- A 3/8-circle body is the most common curvature for skin closure; deeper or confined spaces typically call for a 1/2-circle.
- On the suture pack, more zeros mean a thinner suture, and the letter code after the size is manufacturer-specific shorthand, not a universal standard.
What Is a Needle for Stitches?
A needle for stitches is a curved surgical instrument designed to carry a suture through tissue during wound closure. Most modern versions are pre-loaded with suture and used once per pass.
Every surgical needle has three working zones that shape how it performs:
- Swage: the point where the suture attaches to the needle body.
- Body: the curved section that defines the needle's shape and diameter.
- Point: the tip that penetrates the tissue at the start of each pass.
Surgical needles are sterile, held in a driver, and engineered for specific tissue mechanics. A surgical needle matched to the wrong tissue creates unnecessary trauma at the pass point.
Swaged needles, where the suture is pre-attached to an eyeless body, are the modern standard. The thread sits flush with the needle diameter, so the combination moves through tissue with less drag than an eyed needle carrying a threaded loop, which is why swaged sutures are referred to as atraumatic.
Why Does Choosing the Right Needle for Stitches Matter?
The right needle gives you a cleaner pass through the tissue, a stronger hold on the closure, and a better-looking scar at the two-week check. Point shape, body diameter, and curvature each play a part, and small mistakes on any of them add up across a long incision.
Here's why needle choice matters in everyday practice:
- Tissue Trauma: Taper points required a higher mean tear-through force than cutting points in recent biomechanical testing, pointing to less tearing for delicate tissues.
- Closure Strength: Matching suture size to tissue load keeps the repair from over-stressing or under-supporting the wound.
- Scar Outcome: Finer gauges and reverse-cutting geometry reduce visible track marks in skin closure, especially on the face.
- Closure Time: A mismatched needle slows every pass, and the lost time adds up fast on long incisions.
- Team Safety: Blunt needles significantly reduced glove perforation and needlestick injuries compared with sharp needles in a meta-analysis of 14 randomized trials.
Needle selection is a small decision with big downstream effects, and it's worth a second look before every case type.
What Are the Main Types of Needles for Stitches?
The main types are taper, conventional cutting, reverse cutting, blunt, and spatula, and each is defined by its point geometry. Point geometry determines how the needle enters and passes through tissue, and it's the single most important variable in needle selection. Tissue type drives the choice.
Here's how the common point types compare:

The skin-versus-internal-tissue split drives most selection decisions in everyday surgery, with taper points handling soft tissue and reverse-cutting handling dense outer layers.
Taper Needles in Everyday Cases
Taper points have rounded bodies that narrow smoothly to a sharp tip with no cutting edges. They pierce and spread tissue rather than slicing it, which is why they're the standard for bowel, vessels, fascia, subcutaneous tissue, and tendon repair.
For a needle driver used on delicate internal tissue, a taper is almost always the right load. The geometry minimizes tearing along the pass, which matters most where the tissue itself has little margin for damage.
When Cutting and Reverse Cutting Work Better Than Taper
Cutting and reverse-cutting points carry a triangular cross-section with a third cutting edge. In conventional cutting, that edge sits on the inner (concave) curve. In reverse cutting, it's on the outer (convex) curve. Reverse cutting is preferred for most skin closure because it reduces the risk of the suture pulling through the wound edge under tension.
Recent biomechanical work found that when the puncture force through human skin was measured, point geometry mattered less than needle body diameter in driving the peak force required. That finding nuances the standard teaching, since the needle's diameter often does more work than what the point style suggests.
Where Blunt and Spatula Points Fit
Blunt-tip needles have rounded points and are recommended for fascial closure when reducing needlestick risk to the team is a priority. They pass through fascia and muscle adequately but don't easily penetrate skin, which is the exact property that lowers glove-perforation risk. Spatula needles are reserved for ophthalmic work on sclera and cornea.
How Does Needle Curvature Affect Stitches?
Curvature sets the access angle and the depth of the pass, which determines how the body rotates through tissue before exiting. Shallow curvatures work on accessible surfaces, and deeper curvatures work in confined cavities. Skin closures typically involve a 3/8-circle body, which is the most common curvature in general practice.
The main curvature options and their typical roles are as follows:
- 1/4 Circle: Shallow, highly accessible tissue; common in ophthalmic and microsurgical work.
- 3/8 Circle: The standard choice for skin and superficial closures across most specialties.
- 1/2 Circle: Deep or confined spaces; most general-surgery fascial and visceral work.
- 5/8 Circle: Deep pelvic, oral, and nasal cavities where the rotation room is limited.
- Straight (Keith): Finger-held passes on accessible skin or tendon.
For skin specifically, the curvature decision is nearly always 3/8-circle with a reverse-cutting point. That predictability is also the reason some surgeons are moving past the needle altogether for subcuticular skin closure, where a skin closure suture can be replaced with a faster, more uniform mechanical approach. For instance, SubQ It! removes the needle step entirely by placing dissolving fasteners under the skin.
How Do You Read the Codes on a Suture Pack?
The codes on a suture pack describe the suture size, the needle type, and the suture material. Suture size follows a standard format, where more zeros mean a thinner suture, running from 11-0 at the fine end to 7 at the heavy end.
Here's what each piece of the label typically tells you:
- Suture Size: Numbers like 6-0, 5-0, 4-0, 3-0, 2-0, 0, 1, and 2 describe diameter. A 6-0 is finer than a 3-0; a #1 is thicker than a 2-0.
- Needle Code: Letter codes like CT, SH, FS, and PS are manufacturer shorthand for needle type and size. These codes are proprietary to individual suture brands and aren't standardized across manufacturers.
- Material: Absorbable options include polyglactin 910, poliglecaprone 25, and polydioxanone. Non-absorbable options include nylon and polypropylene. Monofilament versus braided structure is also on the pack.
The codes are worth knowing, but the choice between absorbable sutures and non-absorbable on facial skin may matter less than surgeons often assume. A 2024 meta-analysis covering 804 patients found no statistically significant difference in infection, cosmetic outcome, or wound separation between the two categories on facial closure.
Which Needle for Stitches Matches Which Tissue?
The right needle for any stitch comes down to point type matched to tissue density, and curvature matched to access depth. For most skin work, a reverse-cutting 3/8-circle with a 3-0 to 6-0 suture is the default. For internal tissue, taper points in a 1/2-circle with an appropriate gauge match the repair load.
Here are the pairings most commonly used across general, laparoscopic, and plastic surgery practice:
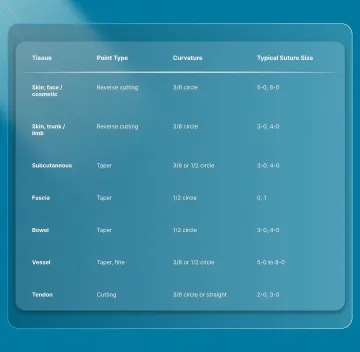

Keeping a quick list like this near the suture cart speeds up selection of the right needles.
When Should You Skip the Needle for Skin Closure?
For planned skin closure where scarring and case time matter, a subcuticular approach without a needle is often faster and cleaner than hand suturing. Subcuticular sutures produce better cosmetic outcomes and higher patient satisfaction than surface staples in abdominal surgery, with similar rates of wound separation.
Hand suturing skin comes with three real costs on every case: it takes longer, the scar depends heavily on the surgeon's hand technique, and non-absorbables need a return visit for removal. Randomized evidence has shown that absorbable subcuticular staples close skin significantly faster than subcuticular suture, with equivalent wound outcomes.

SubQ It! is built for exactly this situation. It places bioabsorbable dermal fasteners under the skin, so the outer skin is never pierced, and there are no railroad-track scar points from staples coming out. The SU-10 handles incisions up to 10 cm, including laparoscopic trocar sites, and the SU-25 covers incisions up to 25 cm on longer open cases.
The fasteners dissolve on their own, so the staple-removal visit goes away, which is relevant to both the patient's experience and a clinic's appointment calendar. A sutureless skin closure approach also produces more consistent closure lines across cases, since the device handles the placement rather than the surgeon's hand technique.
For surgeons closing more than a few skin incisions a week, the time saved adds up quickly. For cosmetic and private-practice plastic surgeons, the cleaner scar line is what patients notice at the follow-up and tell their friends about.
Final Thoughts
Choosing the right needle for stitches comes down to matching point geometry to tissue type, curvature to access depth, and gauge to the load the wound needs to carry.
Reverse-cutting 3/8-circle needles for skin, taper 1/2-circle for deep tissue, and finer gauges where scarring matters. The pack codes describe size, needle, and material. A short reference kept near helps, especially when new procedure types or suture suppliers bring different manufacturer codes into the rotation. Those letter codes don't translate one-for-one across brands, so a written pairing of tissue to point and curvature saves the lookup.
For skin closure specifically, the needle decision doesn't have to be a default. SubQ It! closes the outer skin subcutaneously with bioabsorbable fasteners, cutting closure time and removing the staple-removal visit from the post-op plan. For private-practice surgeons, that time back compounds across a week. Contact us today to request a custom quote.
FAQs
1. What Kind of Needle Is Used for Stitches on the Face?
Facial closure typically uses a reverse-cutting point with a 3/8-circle curvature and a fine suture gauge, most often 5-0 or 6-0. The finer gauge reduces visible needle tracking, and the reverse-cutting edge lowers the risk of the suture pulling through the wound margin.
2. Can You Use a Regular Sewing Needle for Stitches in an Emergency?
Household sewing needles aren't sterile, aren't swaged to suture material, and don't carry surgical point geometry. They're not a safe substitute for a surgical needle outside of the most extreme wilderness scenarios, and any such improvisation creates a significant tissue trauma and infection risk.
3. What Are the Three Main Types of Suture Needles?
The three most common categories are taper, cutting, and reverse cutting. Taper points pierce and spread delicate tissue, cutting points carry a triangular tip for tougher tissue, and reverse-cutting points place the cutting edge on the outer curve to protect skin-wound edges under tension.
4. What Size Needle Is Used for Most Skin Stitches?
Most skin closures on the trunk and limbs use a 3/8-circle reverse-cutting needle paired with a 3-0 or 4-0 suture. Facial and cosmetic cases move to finer gauges like 5-0 or 6-0 to minimize visible tracking and support a cleaner scar at the follow-up visit.
5. Are Swaged Needles Better Than Eyed Needles?
Swaged needles, where the suture is pre-attached to an eyeless body, are the modern standard and are considered atraumatic. The thread sits flush with the needle diameter, so the combination passes through tissue with less drag than an eyed needle carrying a threaded loop.
6. How Do You Hold a Curved Needle for Stitches Correctly?
A curved needle is loaded into the driver at roughly one-third of the way down from the swage toward the point, perpendicular to the driver's jaws. The wrist rotates through the arc of the curve, so the needle follows its own shape through the tissue without torquing.


