
Introduction
A patient with a deep laceration arrives, and repair needs to begin immediately. In these moments, the reliability of a laceration kit directly affects both efficiency and clinical outcomes.
Lacerations account for approximately 8 million) emergency department visits annually in the United States, making them one of the most common injury presentations in acute care.
In practice, variability in kit quality is a recurring challenge. Missing components, poorly aligned instruments, or limited suture options can interrupt workflow and force clinicians to adapt mid-procedure.
This blog outlines what a well-designed emergency laceration kit should include, how to evaluate quality beyond upfront cost, and the common mistakes that impact performance in real-world clinical settings.
Key Takeaways:
- Needle driver performance and scissor sharpness are common failure points that affect closure quality and efficiency.
- Kit-related interruptions often occur due to instrument limitations, not missing components.
- Procurement decisions based solely on unit cost can increase the overall procedural burden.
- Effective kit selection depends on matching components to the actual case mix and workflow demands.
- Maintaining kit reliability requires continuous evaluation based on clinician use, not static checklists.
What is an Emergency Laceration Kit?
An emergency laceration kit is a pre-assembled, sterile collection of surgical instruments, suture materials, and wound care supplies designed for rapid use in repairing traumatic or surgical skin wounds.
These kits standardize care delivery across clinical settings while ensuring all necessary components are immediately available when time matters most.
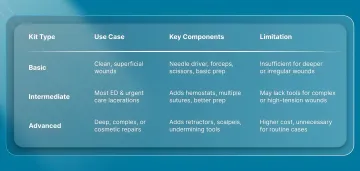
Three Primary Kit Types
The effectiveness of a laceration kit is defined less by its contents and more by how predictably those components perform once the procedure begins.
Breakdowns rarely come from missing items; they come from subtle inefficiencies: inconsistent instrument grip, limited adaptability mid-repair, or packaging that disrupts the natural sequence of use. These include the following kits:
Why Hospitals Use Standardized Emergency Laceration Kits
Even small gaps in kit organization can cost minutes per procedure and increase infection risk. Standardized kits prevent these delays and ensure critical instruments are always ready when seconds matter. Here’s how:
1. Faster Procedural Turnover
Evidence from a quality improvement study in an emergency department showed that using a dedicated laceration supply cart reduced the average repair time from 68.3 minutes to 36.9 minutes, saving roughly 31 minutes per procedure).
- Facilitate faster transitions between cases
- Reduce clinician time spent locating instruments
- Support smoother workflow in busy ED settings
2. Enhanced Emergency Preparedness
Standardized kits ensure all critical instruments and materials are immediately available for unpredictable cases. This reduces mid-procedure improvisation, maintaining sterility and patient safety.
- Immediate access to all necessary components
- Minimize mid-procedure scrambling
- Ensure readiness for complex or high-acuity wounds
3. Data-Driven Inventory Optimization
Tracking kit usage provides actionable insights for stock management. Facilities can reduce waste, avoid overstocking, and prioritize high-demand items, improving both cost efficiency and clinical readiness.
- Identify frequently used versus underused components
- Optimize procurement and reduce unnecessary expenditure
- Support accurate inventory planning
4. Support for Multi-Level Staffing
Pre-assembled kits allow junior, temporary, or rotating staff to perform repairs confidently. Uniform layouts reduce the learning curve and reliance on senior staff during emergencies.
- Simplify procedures for less experienced clinicians
- Maintain consistent quality across staff levels
- Reduce procedural errors due to unfamiliarity
5. Integration With Digital Workflow Tools
Some facilities integrate kit usage data with electronic inventory or procedural logs. This improves compliance reporting, supports audits, and informs strategic supply and staffing decisions.
- Connect kit usage with digital tracking systems
- Enhance operational visibility and reporting
- Facilitate data-driven decision-making
What Makes an Emergency Laceration Kit Effective in Clinical Practice

Beyond just having instruments on hand, a well-designed laceration kit can reveal hidden inefficiencies in procedure flow. Tracking which components are used, skipped, or fail over time helps identify training gaps, optimize kit composition, and prevent unnecessary supply costs insights most EDs never capture.
Essential Instruments
High-quality instruments directly impact repair speed, precision, and safety. Inadequate tools can lead to mid-procedure failures or prolonged procedures.
- Needle driver: Secure needle grip for accurate suturing
- Tissue forceps with teeth: Precise, atraumatic tissue handling
- Suture scissors: Clean, reliable thread cutting without fraying
- Scalpel handle with blade: For wound debridement or revision of irregular edges
Suture Materials
The right suture types prevent re-interventions and support optimal healing.
- Absorbable sutures: (3-0 to 5-0, e.g., Monocryl) for deep layers
- Needle variations: Cutting for skin, tapered for deep tissue
- Poliglecaprone 25 (Monocryl) is the usual best selection for buried sutures
- Non-absorbable sutures: for skin closure.
Wound Preparation Supplies
Proper preparation reduces infection risk and supports faster closure.
- Sterile drapes: Maintain a clean field
- Antiseptic solutions: Chlorhexidine or povidone-iodine
- Sterile gauze: For cleaning and hemostasis
- Local anesthetic with syringes/needles: Ensure patient comfort
Hemostasis and Visualization Tools
Adequate visualization and bleeding control are critical for successful repairs:
- Hemostats/clamps: Control bleeding vessels before closure
- Adequate lighting: Essential for deep or complex wounds
- Retractors: Improve visualization in challenging anatomical locations
Documentation and Safety Items
These components protect both clinicians and patients:
- Sterile marking pens: Wound mapping and measurement documentation
- Specimen containers: Tissue sampling when indicated
- Sharps disposal container: Protects clinicians and patients from needlestick injuries
Optional Advanced Components
Consider adding these items for complex or delicate repairs:
- Skin hooks: Delicate tissue handling without crushing wound edges
- Undermining scissors: Creating tissue planes for tension-free closure
Specialized suture materials: Barbed sutures or tissue adhesives for specific applications
5 Critical Factors for Choosing the Right Emergency Laceration Kit
The right emergency laceration kit ensures reliable performance, efficient procedures, and reduced infection risk. According to the CDC, surgical site infections account for nearly 20% of all healthcare-associated infections, highlighting the critical role of proper instrument quality and sterility.
1. Instrument Quality and Reliability
This is the most critical selection factor. Instrument failure mid-procedure causes delays, requires opening second kits (doubling costs), increases infection risk, and frustrates clinicians.
Quality indicators include:
- Needle drivers: Diamond-cut jaws for secure needle grip
- Scissors: Sharp, aligned blades through hundreds of cuts
- Forceps: Precisely matched teeth for atraumatic tissue handling
Reputable manufacturers with proper quality certifications—such as ISO 13485 registered facilities like those producing advanced closure systems—demonstrate significantly lower failure rates than budget alternatives. This makes quality investment essential for reliable clinical performance.
2. Clinical Setting Requirements
Setting determines kit complexity:
Emergency departments need intermediate-to-advanced kits to handle a wide variety of wounds, from simple lacerations to complex facial repairs requiring specialized techniques.
Urgent care centers typically need intermediate kits for the most common lacerations, though keeping basic and advanced options available ensures appropriate tool availability.
Operating rooms need advanced kits for complex surgical closures, with specialized instruments for plastic and reconstructive procedures.
High-volume settings should consider pre-positioning multiple kit types rather than a one-size-fits-all approach, allowing staff to select appropriate complexity before opening sterile packages.
3. Sterility Assurance and Packaging
Beyond selecting the right instruments for your setting, sterility assurance protects patient safety. Validated sterilization is non-negotiable:
- Ethylene oxide or gamma radiation with clear indicators
- Tamper-evident packaging
- Clear expiration dating
- The manufacturer holds ISO 13485 certification or an equivalent quality management system
4. Consider Cost in Terms of Clinical Impact
Procurement decisions should reflect real-world performance, not just upfront pricing. Poor-quality kits can increase total cost through inefficiencies.
- Factor in instrument failure or replacement rates
- Account for time lost during procedures
- Evaluate the downstream impact on patient throughput
5. Clinician Feedback and Usability
End-user input is critical—procurement decisions made without clinician consultation often fail in practice. Establish a trial period with multiple manufacturers and collect structured feedback on:
- Instrument performance during actual procedures
- Packaging usability and sterile field maintenance
- Component adequacy for typical case mix
- Staff satisfaction and confidence in tools
Common Mistakes to Avoid When Using Emergency Laceration Kits
Even high-quality kits can fail to deliver optimal outcomes if used improperly. This section covers the most frequent errors in purchasing, stocking, and clinical use that compromise patient care.
Prioritizing Cost Over Healing in Procurement
Hospital purchasing departments often select the lowest-bid kits without understanding clinical performance differences. The consequences are predictable: frustrated clinicians, mid-procedure failures, and extended repair times.
Effective procurement strategies:
- Provide purchasing teams with evidence-based quality requirements
- Insist on performance standards in contracts, not just price
- Document failure rates and total cost of poor-quality instruments
- Include clinician input in vendor selection processes
Inadequate Restocking and Expiration Management
Kits expire, get used faster than anticipated, or specific components deplete while others remain, leading to incomplete kits at critical moments. This creates dangerous gaps in emergency preparedness.
Solution framework:
- Implement par-level systems with automated reordering
- Conduct monthly expiration audits
- Track usage patterns to optimize kit composition
- Assign specific staff responsibility for inventory management
Failing to Match Kit to Wound Complexity
Using a basic kit for a complex wound leads to mid-procedure scrambling for additional supplies, breaking the sterile field, and prolonged repair times. This wastes time and increases infection risk.
Best practice: Train staff on rapid wound assessment and appropriate kit selection before opening sterile packages. Create simple decision trees based on wound characteristics to guide selection.
Skipping Instrument Inspection Before Use
Even quality kits can have occasional defects. Opening the kit and immediately starting without inspecting the instruments can lead to discovering problems after the patient is prepped.
30-second instrument check:
- Needle driver jaw alignment and grip strength
- Scissors sharpness and blade alignment
- Forceps teeth alignment and closure
- Packaging integrity and sterility indicators
Not Considering Modern Closure Alternatives
Many facilities stock only traditional suture-based kits without evaluating newer closure technologies that may improve outcomes for specific cases. Traditional laceration kits remain essential for traumatic wounds and emergency presentations.
However, surgical settings performing planned procedures can benefit from incorporating advanced closure technologies. For high-volume facilities performing abdominal, thoracic, gynecologic, orthopedic, or plastic procedures, bioabsorbable subcuticular systems like SubQ It! offer compelling advantages.
These systems reduce closure time significantly compared to manual suturing. They eliminate staple removal appointments and improve cosmetic results for appropriate surgical incisions.
Smarter, Faster, Safer Wound Closure with SubQ It!

While emergency laceration kits remain essential for traumatic wounds and ED presentations, planned surgical settings operate under different constraints and can benefit from advanced closure technologies.
SubQ It! is a bioabsorbable subcuticular skin closure system that addresses limitations of both traditional sutures (time-consuming) and metal staples (poor cosmesis, require removal) for surgical incisions.
- Rapid, Subcuticular Closure: Deploys bioabsorbable fasteners in ~7 seconds each, achieving closure up to 7× faster than manual sutures in laparoscopic and other surgical incisions.
- Two Size Options: Available in SU‑10 (up to ~10 cm) and SU‑25 (up to ~25 cm) configurations for short and longer incisions.
- No Removal Needed: Fasteners are bioabsorbed after healing, eliminating staple removal visits and patient discomfort.
- Cosmetic Advantage: Subcuticular placement avoids external skin penetration and “train‑track” scarring typical of metal staples.
- Safety Features: Built‑in retractable needles and stop mechanisms reduce needlestick risk during deployment.
- FDA Cleared & ISO Certified: Registered under FDA 510(k) clearance K131563 and manufactured under ISO 13485 quality systems.
Final Thoughts
Emergency laceration kits do more than hold instruments; they simplify workflow, reduce procedure delays, and safeguard patient outcomes in every clinical setting. High-quality, well-stocked kits ensure sterile, reliable closure for both simple and complex lacerations.
Traditional sutures remain critical for deep or high-tension wounds, while bioabsorbable subcuticular systems like SubQ It! complement them in planned procedures. By enabling precise subcuticular closure, reducing the need for external staples, and supporting superior wound closure outcomes, they help surgical teams save time and improve patient satisfaction.
Incorporating tiered kit strategies, routine audits, and clinician feedback ensures optimal performance, reduces mid-procedure disruptions, and enhances both safety and efficiency. Explore how SubQ It! fits into your workflow to elevate surgical outcomes and patient care.
Frequently Asked Questions
1. What is a laceration kit?
A laceration kit is a pre-assembled, sterile package containing surgical instruments (needle driver, forceps, scissors), suture materials, and wound preparation supplies for repairing skin wounds in emergency settings.
2. What are the 4 C's of wound care?
The 4 C's framework consists of: Cleaning (irrigation and debridement), Closing (appropriate closure method selection), Covering (sterile dressing), and Checking (follow-up assessment for infection or complications).
3. What instruments are essential in a laceration kit?
Core instruments include: needle driver (for suture placement), tissue forceps with teeth (for tissue handling), suture scissors (for cutting thread), and a scalpel handle with blade (for debridement).
4. How often should laceration kits be restocked and inspected?
Conduct monthly expiration date audits, replace immediately after use, perform quarterly usage pattern analysis to optimize par levels, and complete semi-annual clinician feedback reviews to ensure kit contents meet evolving clinical needs.
5. What's the difference between basic and advanced laceration kits?
Basic kits contain 3-5 essential instruments for simple repairs, intermediate kits include 6-8 instruments for most ED/urgent care needs, and advanced kits feature 10+ instruments with specialized tools (skin hooks, undermining scissors) for complex surgical closures.


