Introduction
Wound closure is a defining step in surgery where technique selection directly influences tissue handling, healing outcomes, and operative efficiency. The decision between stitches or staplers is a routine yet important consideration across many surgical procedures.
Sutures allow controlled, adaptable approximation of tissue, making them suitable for layered closures and anatomically delicate regions. Staplers, on the other hand, enable rapid and consistent closure, particularly in long incisions where speed is clinically relevant.
Choosing between the two is not about preference but procedural suitability. This blog breaks down stitches and staplers in terms of mechanism, clinical applications, and evidence-based considerations to support informed surgical decision-making.
TL;DR
- Both stitches and staplers achieve comparable wound healing outcomes, with no consistent evidence of superiority in routine surgical closure.
- Selection is procedure-dependent, based on incision length, tissue tension, anatomical site, and required level of precision or speed.
- Staplers are primarily used for efficiency, offering rapid closure in long incisions and reducing overall operative time.
- Sutures are preferred when precision is critical, especially in layered closure or anatomically or cosmetically sensitive regions.
- Clinical differences in infection risk, pain, and scarring are inconsistent, with outcomes more influenced by surgical technique and patient factors than closure method.
What Are Stitches (Sutures)?
Stitches (sutures) are sterile threads used to close wounds by bringing tissue edges together until natural healing occurs. They are one of the most established methods of wound closure and are used across a wide range of surgical procedures.
Sutures function as a temporary support system, maintaining wound approximation and reducing tension while the tissue regains strength.
They are broadly classified based on material and behavior:
- Absorbable sutures: Gradually broken down by the body; absorbable sutures are commonly used for internal or deep tissue closure
- Non-absorbable sutures: Retain strength longer and may require removal; often used for skin or high-tension areas
What Are Staplers (Skin Staplers)?
Skin staplers are mechanical devices used to close wounds by placing sterile metal staples across the skin edges. They provide rapid and uniform approximation of tissue, making them especially useful in procedures where speed and efficiency are critical.
Common staple materials include:
- Titanium: widely used due to high biocompatibility, corrosion resistance, and low tissue reactivity; generally MRI-safe.
- Stainless steel: high tensile strength for secure closure; may cause nickel sensitivity in some patients.
- Bioabsorbable polymers (e.g., polylactide/polyglycolide-based): degrade in vivo, eliminating or reducing the need for removal.
Staplers are not a replacement for sutures, but a situational tool chosen based on surgical context and procedural efficiency needs.
9 Clinically Proven Differences: Stitches vs Staplers
Sutures and staples are both standard techniques for surgical wound closure, with extensive clinical evidence showing broadly similar outcomes in healing, infection risk, and patient satisfaction. Differences are primarily related to speed of closure, technical control, and procedure-specific suitability rather than overall effectiveness.
The table below summarizes the key differences across relevant clinical dimensions:
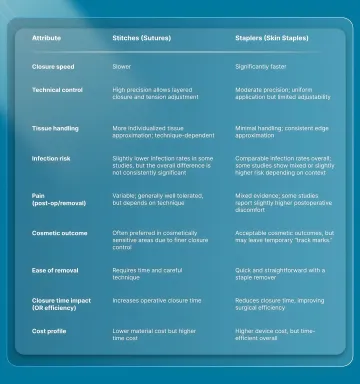
When Are Stitches vs Staplers Preferred in Surgical Practice?
Following are the common situations where surgeons typically choose one method over the other:
Stitches (Sutures) are typically preferred for:
- Facial and cosmetically sensitive areas, where precise edge alignment and minimal scarring are critical
- Small or delicate wounds that require fine control over tissue approximation
- Layered closures, where deeper tissue and skin need to be closed separately for optimal healing
- Patients with higher cosmetic priority or sensitive skin, where controlled tension distribution improves outcomes
Staplers are typically preferred for:
- Large surgical incisions, especially in abdominal or orthopedic procedures where rapid closure is needed
- Emergency and trauma settings, where reducing operative time is clinically important
- High-tension or high-movement areas, such as the scalp, back, or limbs
- Situations where speed and consistent wound approximation outweigh cosmetic refinement
SubQ It!: A Subcuticular Bioabsorbable Skin Closure System

Traditional metal staples allow fast skin closure but involve external placement, removal within 7–10 days, and the risk of linear “railroad-track” scarring. SubQ It! uses bioabsorbable subcuticular fasteners placed beneath the skin that gradually resorb, eliminating the need for removal and supporting improved cosmetic outcomes.
- Subcuticular bioabsorbable closure: Uses absorbable fasteners placed beneath the skin to maintain wound approximation during healing. The material gradually dissolves over time, eliminating the need for removal.
- No removal requirement: Designed to avoid external removal procedures by using internal, absorbable fixation instead of external metal staples.
- Subcutaneous placement approach: Fasteners are positioned below the skin surface, avoiding external exposure and relying on internal wound support during healing.
- Applicability across incision lengths: Can be used across a range of incision sizes, including small laparoscopic port sites as well as longer surgical incisions, depending on device configuration.
- Device variants:
- SubQ It! 10: intended for closures up to 10 cm, typically small or laparoscopic incisions
- SubQ It! 25: intended for closures up to 25 cm, used for longer surgical incisions
Final Thoughts
Stitches and staplers both serve the core purpose of wound closure, but their value depends entirely on surgical context, tissue type, and procedural priorities.
Sutures provide precision and adaptability, making them suitable for layered closure, delicate tissues, and areas where cosmetic alignment is important. Staplers prioritize speed and consistency, making them ideal for long incisions and situations where reducing operative time is critical.
For workflows where speed, reduced surface trauma, and predictable closure are key, SubQ It! offers a bioabsorbable stapling approach designed for efficient subcuticular closure without removal, helping streamline postoperative care while maintaining closure strength in appropriate indications.
To explore how SubQ It! can integrate into your surgical practice, connect with the SubQ It! team.
FAQs
1. Which is better for surgical wound closure: stitches or staples?
Neither method is universally superior. Stitches (sutures) and staplers have broadly comparable clinical outcomes in terms of wound healing. The choice is typically guided by surgical context, incision length, anatomical site, and intraoperative priorities rather than the inherent superiority of one method.
2. Do stitches heal better than staples in surgery?
Both achieve effective wound approximation when properly applied. Sutures may offer finer edge control in select cases, while staplers are often preferred for speed in longer incisions.
3. Are staples associated with a higher risk of infection than stitches?
The evidence is mixed and not definitive. Some studies report a slightly higher incidence of superficial wound infection with staples, while others find no significant difference. Overall, infection risk is more strongly influenced by wound contamination, operative time, and patient factors than by closure method alone.
4. Do staples leave worse scars compared to stitches?
Staples may produce more visible track marks in the early healing phase, but long-term cosmetic outcomes are often comparable between staples and sutures. Sutures are generally preferred in cosmetically sensitive areas where precise edge approximation is required.
5. Why do surgeons choose staplers instead of stitches?
Staplers are primarily used for efficiency. They significantly reduce wound closure time, which can shorten overall operative duration and reduce time under anesthesia. They are particularly useful in large, straight, or high-tension incisions, such as abdominal or orthopedic surgeries.
6. Can I ask for stitches instead of staples?
You can discuss preferences with your surgeon, but the final decision should prioritize clinical factors like wound characteristics and optimal healing. Your surgeon's expertise will determine the most appropriate closure method for your specific case.
7. Are staplers faster than stitches in clinical practice?
Yes. Staplers are consistently faster than suturing, especially in long incisions. This time advantage is clinically relevant in high-volume surgeries or situations where minimizing anesthesia duration is important.