
The closure technique directly influences how the wound is supported, how long the case runs, and what steps follow surgery.
Studies comparing closure methods report average times of roughly 7.17 minutes for staples and around 13.93 minutes for sutures. This difference highlights the measurable impact of technique choice on operating room efficiency.
For this reason, suture staple guns are frequently selected for their speed. However, their external placement and the need for removal influence how closure is managed after surgery.
In this blog, you’ll explore how surgeons evaluate suture staple guns in 2026, including their clinical trade-offs, workflow impact, and comparison with sutures.
Key Takeaways:
- The term “suture staple gun” is non-clinical and typically refers to skin staplers used to rapidly close external wounds.
- Sutures offer greater control over tissue approximation, while staplers provide faster, more consistent closure.
- External skin staplers introduce trade-offs, including visible skin penetration, the need for removal, and an added postoperative workflow.
- Closure technique directly influences operative time, with staples showing a clear time advantage over sutures.
- Closure method selection depends on incision length, wound tension, cosmetic priorities, operative time, and follow-up requirements.
What Is a Suture Staple Gun in Surgical Closure?
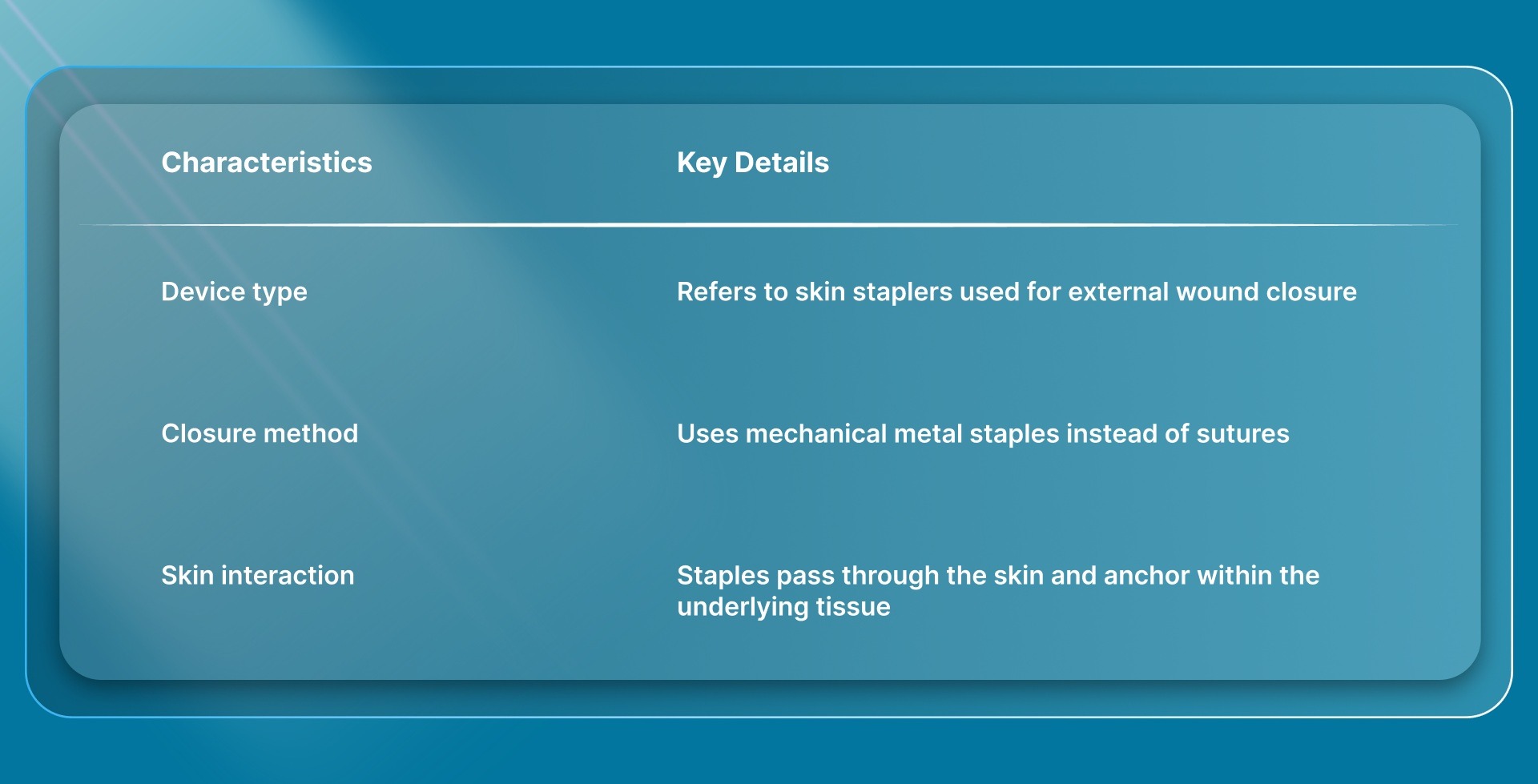
A “suture staple gun” is not a clinical term. It typically refers to skin staplers used to rapidly close surgical incisions.
In practice, closure is done using sutures or skin staplers. Sutures use needle-and-thread for controlled tissue approximation, while staplers place metal staples through the skin to close wounds more quickly.
Each staple is formed beneath the skin surface to hold wound edges together, remains externally visible, and is removed after healing, depending on the incision site.
Once you understand what a suture staple gun is, it also provides useful context for clarifying how closure technique differs when comparing sutures and skin staplers.
Sutures vs Skin Staplers: What Changes in Closure Technique
The difference between sutures and skin staplers is how tissue is approximated, controlled, and managed after closure. At the point of closure, the choice is between manual precision and mechanical consistency.
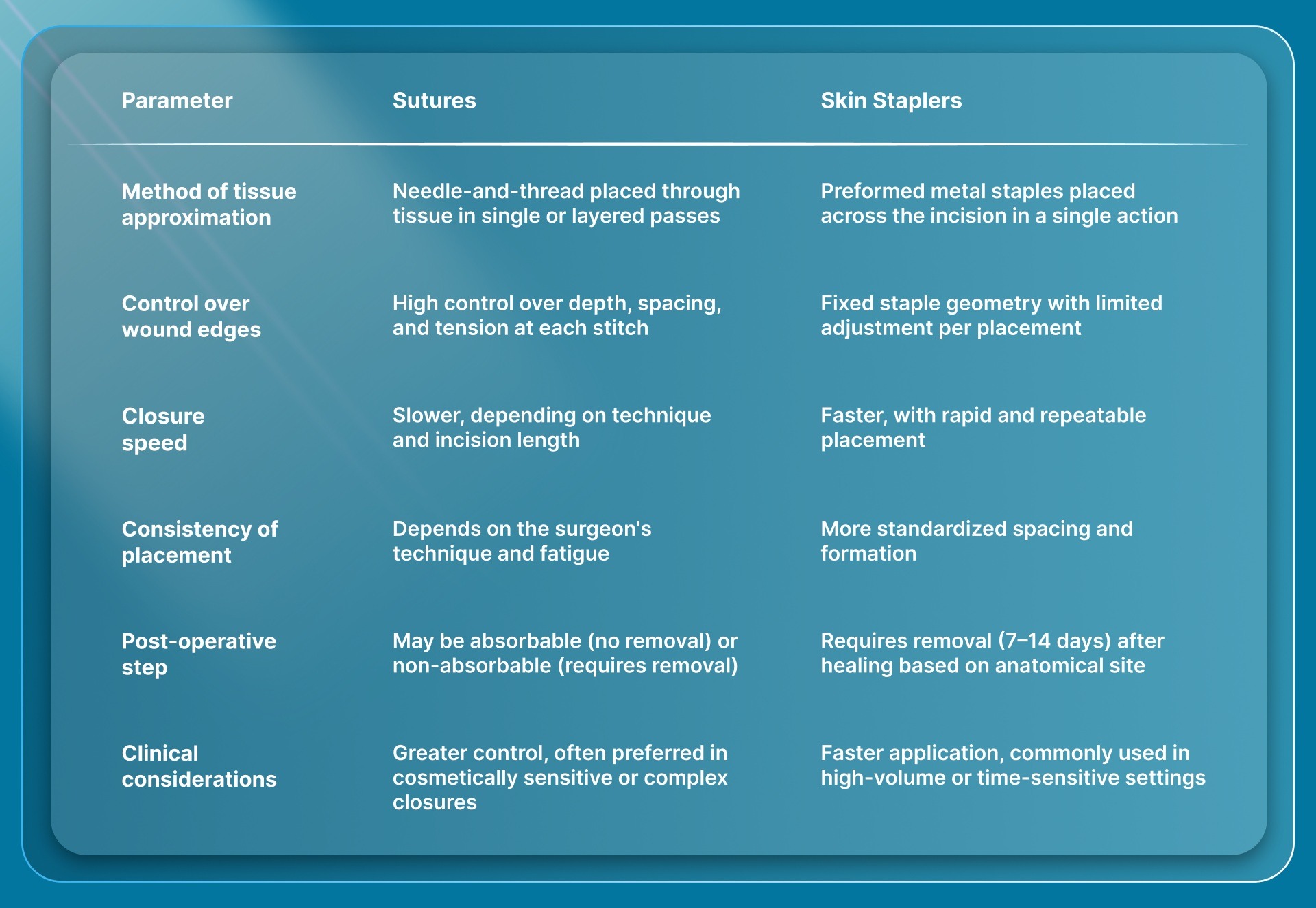
In practice, the choice comes down to balancing control during closure with efficiency in the operating room.
As incision length increases and closure time becomes more significant, approaches such as SubQ It! SU-25 uses subcuticular, device-based deployment to maintain internal approximation while improving speed.
The differences in closure technique also help explain why various types of suture staple guns have been developed for specific surgical needs.
Types of Suture Staple Guns You Should Know
In surgical practice, closure devices used in place of sutures vary by how the fasteners are applied and where they are used in the closure process. For skin closure, these fall into two clinically relevant categories.
1. Traditional Metal Skin Staplers
These are the most widely used devices for external skin closure across surgical settings. They are typically selected when speed and simplicity are the primary priorities.
- Manual trigger-based devices: Each activation deploys a metal staple across the incision
- Common in routine and high-volume cases: Used across general surgery, orthopedics, trauma, and emergency settings
2. Bioabsorbable Subcuticular Stapling Systems
These systems represent a different approach to closure, placing fasteners within the dermal layer rather than across the skin surface. They are used when the closure technique differs from traditional external stapling.
- Designed for subcuticular closure: Used in procedures where internal dermal approximation is preferred
- Applicable across incision sizes: Used in both smaller and longer incisions, depending on the system and technique
Understanding the available types also highlights the practical trade-offs that external skin staplers can introduce in clinical practice.
Where External Skin Staplers Create Trade-Offs in Practice?
External skin staplers are widely used because they simplify closure and reduce operative time. In practice, that speed introduces trade-offs that affect wound appearance, follow-up workflow, and control during closure.
These trade-offs include:
- External skin penetration: Staples pass through the epidermis and remain visible on the surface, creating multiple puncture points along the incision
- Cosmetic variability: Outcomes depend on placement and removal timing and may result in visible “railroad-track” marks
- Mandatory removal step: Staples require removal after healing, adding a follow-up visit, staff time, and coordination
- Dependence on removal timing: Early removal can reduce wound support, while delayed removal may increase visible marking
- Limited adjustment during placement: Fixed staple geometry offers less control over tension and edge alignment compared to suture-based techniques
- Shift in workflow beyond closure: Faster intraoperative closure is offset by additional post-operative management.
Recognizing the trade-offs associated with external skin staplers also informs the broader decision of selecting the most appropriate closure method for each procedure.
How to Choose the Right Closure Method for Each Procedure?
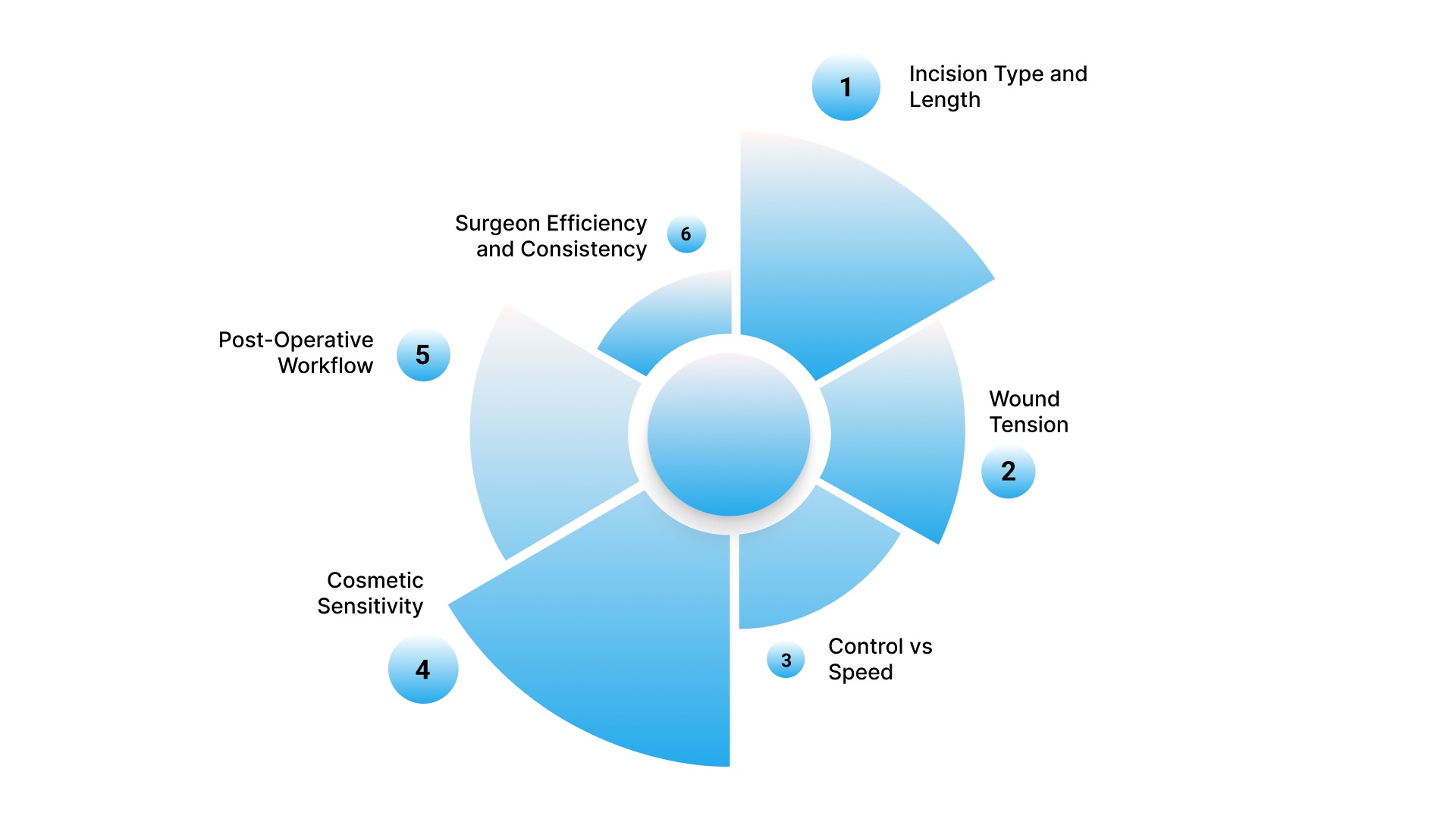
Choosing the right closure method is a procedure-specific decision based on incision characteristics, tissue behavior, and post-operative requirements. The aim is to balance control during closure, operative time, and follow-up workflow.
1. Incision Type and Length
Incision size influences how closure is approached. As incision length increases, the need often shifts from precision to efficiency.
- Short incisions often benefit from controlled placement: Smaller wounds typically require precise approximation to maintain alignment in limited space.
- Long incisions benefit from efficient closure methods: Larger wounds often favor faster, repeatable techniques to reduce overall closure time.
2. Wound Tension
Tension across the wound determines how much support and control the closure must provide. Higher tension increases the need for careful approximation.
- High-tension wounds require greater control: These areas often need techniques that allow adjustment of depth, spacing, and tension.
- Low-to-moderate tension allows more flexibility: These wounds can often be closed with methods that prioritize speed and consistency
3. Control vs Speed
Closure methods differ in how they balance precision and efficiency. The decision depends on the procedural priorities for that case.
- Sutures provide controlled approximation: They allow adjustment of tissue depth, spacing, and edge alignment throughout closure
- Stapling systems provide faster deployment: They enable rapid, consistent placement across the incision
4. Cosmetic Sensitivity
The location of the incision affects how much emphasis is placed on the final appearance. Outcomes can vary depending on technique and procedure type.
- Visible areas often require precise edge alignment: Greater control during closure helps optimize scar appearance
- Covered areas may allow faster closure methods: Cosmetic considerations are typically lower, allowing efficiency to take priority
5. Post-Operative Workflow
The selection of closure methods directly affects what happens after surgery. Some approaches introduce additional follow-up steps.
- Methods requiring removal add follow-up burden: These involve additional visits, staff time, and coordination
- Methods that do not require removal simplify recovery: Eliminating removal reduces post-operative handling
6. Surgeon Efficiency and Consistency
The chosen method must be reliable under real operating conditions. Consistency becomes critical when used repeatedly across cases.
- Familiar techniques improve execution consistency: Surgeons tend to perform more efficiently with methods they use regularly
- Standardized systems reduce placement variability: Mechanical deployment helps ensure uniform spacing and formation across the incision
Final Thoughts
Closure decisions extend beyond the incision, shaping case efficiency and post-operative management across procedures. As case volume increases, these effects become more visible in overall workflow and scheduling.
In this context, SubQ It! SU-25 is designed for longer incisions, using 25 bioabsorbable fasteners to support closure of up to 25 cm while reducing closure time by approximately 25 minutes per case.
This becomes particularly relevant in private practice settings where operative time directly impacts case throughput.
Contact us today to learn how SubQ It! SU-25 can fit into your closure workflow and support more consistent, efficient outcomes.
FAQs
1. Can a skin stapler be used for every type of incision?
No. The choice depends on factors such as incision length, wound tension, anatomical location, and cosmetic requirements. In many cases, surgeons may prefer sutures or subcuticular techniques where greater control or aesthetic precision is needed.
2. Are skin staplers used only in the operating room?
No. While they are commonly used in the operating room, skin staplers are also used in emergency and trauma settings where rapid closure is required. Their use depends on the clinical context and the need for speed versus control.
3. Do surgical staples affect post-operative imaging?
Surgical staples are generally safe for imaging, including MRI, and do not pose safety risks in most cases. However, they may create localized artifacts near the closure site, which can affect image clarity depending on the material and location.
4. What training is required before using a skin stapler?
Skin staplers require basic device-specific training to ensure proper placement, spacing, and removal. Correct technique is important for maintaining consistent wound approximation and reducing the risk of complications.
5. Can skin staplers be used as part of a layered closure?
Yes. Skin staplers are often used for surface closure after deeper layers have been approximated with sutures. This approach helps manage wound tension while maintaining efficiency during the final stage of closure.
6. What factors should be evaluated before selecting a closure method?
Surgeons typically assess incision type, wound tension, cosmetic considerations, operative time, and follow-up requirements. The decision is based on how the closure will perform both during the procedure and throughout the healing process.


